Paul Licina and Emma Johnston
PATHOPHYSIOLOGY
The diagnosis of reherniation is often accompanied by the question ‘why did this occur?’ Natural human instinct is to seek an external traumatic cause rather than implicating intrinsic factors within the disc itself. Nevertheless, both causes are relevant, the latter likely more so. Currently, the importance of intrinsic factors in disc degeneration and herniation is gaining momentum at the expense of a focus on external factors. However, the factors that lead to reherniation, whether external or internal, are likely somewhat different than those that led to the initial herniation.
Factors Influencing Reherniation
Patient characteristics
Previous research has identified a number of risk factors for disc herniation including age, sex, smoking, diabetes and obesity. However, there is a lack of consensus. A recent meta-analysis found that smoking and diabetes were the main predictors for recurrent disc herniation.1 Increased BMI has also been commonly cited,2-4 with one study reporting that obese patients (BMI ≥ 30) were 12 times more likely to suffer a reherniation than non-obese patients.5 While most studies found that risk increased with age, the SPORT study found that younger age was an independent risk factor.6 Extrinsic factors such as occupation have not been found to be relevant in recent research.1
Radiological parameters
Increased disc height and segmental motion, and increased lumbar lordosis are strong predictors of recurrence. There is also a correlation with recurrence and lower Pfirmann grade (3 vs. 4) and the presence of Modic I end-plate changes.3
Morphology of original herniation
The nature of the original herniation influences the risk of reherniation. Broadly there are two types of herniation: a protrusion where the annulus is stretched but still partly intact, and an extrusion (or sequestration) where the annulus has a discrete defect. A discrete post-extrusion lesion may be able to heal more effectively than the stretched and thinned post-protrusion annulus. It may be that after a protrusion, there is the potential to reherniate at a different point in the weakened annulus whereas after an extrusion or sequestration, reherniation is most likely through the original defect.
The size of the annular defect has been correlated with the risk of recurrence. Carragee et al. found that an annular defect measuring more than 6 mm had a recurrence rate of 27%, compared with 1% for a small annular defect.7 However, other studies have not confirmed a difference of this magnitude.8
Surgical technique
Different surgical techniques are referred to in the literature but there is lack of clarity regarding the exact nature of these techniques. The traditional procedure was a standard discectomy, developed before imaging techniques could reliably identify the location of the herniation, and involved an extensive exposure, a two-level hemilaminectomy and aggressive removal of the disc with curettage of the endplates. Microdiscectomy was first described in 1977 by Caspar,9 who advocated a less invasive technique using a microscope, a small skin incision and a single level fenestration, but with incision of the annulus and subtotal disc removal including the nucleus down to healthy cartilaginous endplates. This has been referred to as subtotal discectomy. Williams10 described a similar technique in 1978 but with no bone removal, blunt annular perforation and removal of only those fragments that are easily mobilised. This concept has been referred to by others as a sequestrectomy or fragmentectomy, the latter term being more inclusive as it applies to both sequestrated and loose extruded disc fragments. A true fragmentectomy does not require opening the annulus, and the disc space is not entered.11,12 Thomé et al.12 expanded the definition of the fragmentectomy technique to include subligamentous extrusions, as well as transannular extrusions where the herniation is still in continuity with the disc space and has only partially passed through the annulus. In these cases, the posterior longitudinal ligament or outer annulus is perforated with a blunt instrument to allow access to and removal of the herniation. Again, the disc space is not entered, and only free fragments and tissue that can be easily mobilised from the intervertebral space are removed. These technique variations need to be kept in mind when reviewing the literature, as many articles provide scant detail regarding the actual technique, and metanalyses may well combine different techniques.
There are conflicting thoughts regarding the difference in outcome between aggressive discectomy and fragmentectomy. It was traditionally thought that removal of most of the nucleus would minimise the risk of recurrence. Indeed, earlier studies showed a greater risk of herniation with fragmentectomy, with Caragee et al. finding a rate of 18% with sequestrectomy compared to 9% with subtotal discectomy.7 A more recent study of 172 patients found a recurrence rate of 15% with sequestrectomy and only 6% in aggressive discectomy.11 In contrast, other studies show that fragmentectomy does not have a higher reherniation rate, but that aggressive discectomy is associated with poorer satisfaction, greater loss of disc height13 and a higher level of recurrent back pain.14,15
Aggressive disc clearance and, to a lesser extent, resection of a protrusion, requires an annulotomy, whereas a fragmentectomy for extrusion or sequestration requires little or no annular incision. The creation of an annulotomy is likely to increase the risk of reherniation, especially if a rectangular section of annulus is removed for access rather than utilising a cruciate incision.
One method to avoid entering the disc while minimising the risk of retained loose fragments is to lavage the disc space. A study by Ellenbogen et al. demonstrated a trend towards a lower rate of recurrence with this technique.16
Postoperative activity
It was previously thought that patients should delay their return to normal activity after discectomy as this would allow the disc to heal and reduce the chance of a reherniation. However, there are few findings to support this and strong evidence that early return to normal activity is beneficial rather than harmful. Studies have shown that removing postoperative restrictions and allowing immediate return to activity and exercise leads to earlier return to work and does not correlate with an increased rate of revision surgery.17-19 It is logical to restrict activity only until the wound has healed.
INCIDENCE
It is important to remember that i) not everyone who has recurrence of symptoms has a reherniation, ii) not everyone who has a reherniation is symptomatic, iii) not everyone who has a symptomatic reherniation needs surgery, and iv) not everyone who has surgery has a revision discectomy. This has significant bearing on data presented in the literature.
An acceptable definition of a recurrence is where all of the following conditions apply to a disc reherniation: i) at the same level and same site as the previous herniation, ii) within two years of a primary discectomy, iii) after a period of symptomatic improvement, iv) in the presence of recurrent concordant radicular symptoms and signs, and v) confirmed with appropriate imaging. Some stipulate that the pain-free period must be at least six months, but the rationale of this arbitrary cut-off is questionable, especially considering that symptomatic reherniation occurs in many patients within the first six months. Our cut-off of two years maximum is equally as arbitrary, but most recurrences occur within this period20 and it may be advantageous to have an end-point to allow comparison of data.
Variability with the definition can occur regarding i) whether the recurrence is symptomatic, ii) whether the recurrence is located at the same level and on the same side, iii) how much time has elapsed since the primary discectomy, and iv) the nature of the imaging that confirmed the recurrence. These factors should be considered when interpreting and comparing studies regarding recurrence.
Incidence of Reherniation
The rate of reherniation varies in the literature from 1% to over 20%,14,15,21 with an accepted rate of 5–10%. If MRI is performed routinely after discectomy, it shows a high rate of asymptomatic recurrence. One study showed a radiographic recurrence rate of 23% within two years, with only 10% being symptomatic.22 In this study, no patient demonstrated residual disc on immediate postoperative MRI and recurrence usually occurred by 12 months. However, earlier studies have shown pseudodisc present on immediate postoperative MRI in 80–95% of patients,23,24 with no correlation with symptoms and gradual resolution over time. This may be attributable to the inferior imaging quality of MRI scans at the time of the studies.
Incidence of Reoperation
The reoperation rate in a large metanalysis was similar to the reherniation rate (5.5% vs. 5.2%),15 suggesting that the majority of recurrences progress to reoperation. The majority of reoperations are revision discectomies, but about 5% are fusions.21
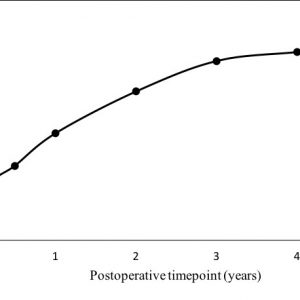
The authors’ long-term prospectively collected audit data with regard to revision discectomy for symptomatic recurrence is presented in Table 2-1. This data shows the revision rate to be within the range quoted in the literature. Figure 2-1 plots the cumulative revision rate and demonstrates that it rapidly rises in the first six months, increases more gradually until two years and then rises quite slowly thereafter.
| Time Post-surgery | Primary Discectomies | Revision Surgeries | Revision Rate |
|---|---|---|---|
| 6 weeks | 1112 | 17 | 1.5% |
| 3 months | 1112 | 13 | 2.7% |
| 6 months | 1112 | 7 | 3.3% |
| 1 year | 1112 | 16 | 4.8% |
| 2 years | 1014 | 19 | 6.6% |
| 3 years | 885 | 12 | 8.0% |
| 4 years | 754 | 3 | 8.4% |
| 5 years | 639 | 2 | 8.7% |
There is little data on the incidence of multiple recurrences, and the best estimate of the authors is that the risk of a second recurrence is similar to that of the first recurrence. While the majority of reoperations are revision discectomies, re-recurrences are more likely to be treated with a fusion. Additionally, persistent symptoms even in the absence of a definite recurrence may lead to further surgery. A review of a national insurance billing database revealed a 4-year reoperation rate of 12%, with the percentage of those undergoing revision discectomy subsequently undergoing fusion at 4 years being nearly 40%.25
DIAGNOSIS
Clinical Presentation
The clinical presentation may not be as clear as with a primary disc herniation for a number of reasons. The first is that there may be residual symptoms and signs from the primary disc herniation, including radicular pain, numbness and reflex loss. The next is that there may be symptoms and signs arising from the discectomy surgery and its consequences, including discogenic low back pain and referred lower limb pain. It may be difficult to distinguish these clinical features from a recurrence of the radiculopathy associated with reherniation. The longer and more complete the pain-free interval between surgery and recurrence, the more one can assume there has been some structural change causing new neural irritation.
Symptoms
Some patients report similar symptoms to those experienced with the original herniation. However, many note a difference in the location, severity or type of pain. They may describe a change in aggravating activities or positions and might report a difference in the presence or degree of sensory disturbance or weakness. The degree of associated back pain can also vary. Presumably the difference arises as a result of nerve root tethering from postoperative epidural fibrosis, as well as a difference in the size or direction of migration of the recurrence.
Signs
The signs found on examination may not be as typical of a radiculopathy associated with a primary disc herniation. Nerve root compression signs (e.g., weakness, paraesthesia) and tension signs (i.e., straight leg raise) may not be affected as much as expected considering the degree of pain reported. Differences can be attributed to nerve root tethering with inability for the nerve to move away from the reherniation.
Injection
If the clinical picture is unclear, diagnostic CT-guided selective nerve root injection with local anaesthetic with or without steroid may be useful. Relief of at least 80% of symptoms for at least 6 hours within an hour of the nerve root block can be considered a positive result, and suggests that the pain is radicular rather than referred.
Imaging
CT scan
CT is notoriously unreliable after previous spinal surgery. It incompletely distinguishes between scar and recurrence because, although herniated disc material shows at a higher range of attenuation than fibrosis, the attenuation ranges for both overlap. Whilst of limited use for diagnosis, it can show bony changes of previous surgery clearly and may assist in surgical planning. Its use is decreasing with the increased awareness of the risks of ionizing radiation and iodinated contrast material.26
MRI scan
MRI is the mainstay for diagnosis of recurrent disc herniation. The imaging protocol should include T1-weighted and T2-weighted sequences in the axial and sagittal planes as well as contrast-enhanced T1-weighted sequences. The administration of gadolinium assists in distinguishing a recurrent disc herniation from postoperative fibrosis by enhancing areas of granulation tissue. The accuracy of these images is increased by adding fat saturation. This negates the signal from normal epidural fat and accentuates the appearance of any enhancing tissue. The post-discectomy spine displays a number of findings on MRI that are considered normal, and that vary depending on how much time has elapsed after surgery.27 In the acute postoperative spine, there is commonly a thin band of enhancement along the surgical track and into the laminectomy or laminotomy. This commonly extends around the thecal sac on the side of surgery, and into the anterior epidural space. There is also usually enhancement of the annular defect within the disc. As postoperative scarring matures from 3 to 6 months, the enhancement in the posterior tissues usually subsides. At this stage, the epidural scar will be seen as a rim of low to intermediate signal material replacing the normal high signal epidural fat on T1 and T2 weighted images. This material usually partly encircles the thecal sac and may surround nerve roots. There should be no, or minimal, mass effect with neurological structures surrounded, but not displaced or distorted. Epidural scar enhances uniformly with gadolinium.28
Recurrent disc is usually seen as a round to ovoid mass in the anterolateral epidural space. It is usually low signal on T1 and T2 weighted images and is contiguous with the underlying disc, unless sequestrated.29 The most common appearance post-gadolinium is a thin rim of enhancement surrounding the disc due to granulation tissue. Less commonly, there is no enhancement. These enhancement characteristics are the most reliable MRI sign that distinguishes a recurrent disc from an epidural scar.30
PREVENTION
Annular Closure
It is understood that the annulus is an avascular structure with a limited capacity for healing. This process is slow and there is thought to be an increased risk of reherniation while it is occurring. Many attempts have been made to establish an effective means by which to close the annular defect at the time of surgery to prevent this risk of reherniation. Various techniques including the use of collagen gels, sutures and devices have been developed and while some have shown promise, closing this defect remains a surgical challenge.31
TREATMENT
Observation
Expectant treatment is the mainstay in the early stages of symptomatic disc herniation. In the opinion of the authors, definitive intervention should be considered earlier in recurrent herniations as spontaneous resolution seems less common than with primary herniation. This premise is supported by the fact that the rate of symptomatic recurrence is very similar to the rate of reoperation. The explanation may be that postoperative epidural fibrosis inhibits the natural resorptive process.
Physical Therapies
While playing a role in symptom management and improvement of function, physical therapies have not been shown to alter the natural history of disc herniation.32 There is no reason to believe that this is not also the case for recurrent herniations.
Steroid Injections
Epidural steroid injection is an accepted and effective treatment for disc herniation.33 A study of recurrent herniation showed that epidural steroid injection via the caudal and transforaminal routes showed similar effects in terms of pain and patient function, although the response was less than that in primary herniations, presumably due to epidural fibrosis limiting the spread of injectate.34
Surgery
Indications
The indications for surgery are similar to those for primary discectomy, but the decision to proceed may be less clear as it is often more difficult to make a firm diagnosis. The clinical findings are less precise and there is a high rate of false positive findings on MRI. This may mean that one proceeds with surgery but no herniation is found. The fact that revision surgery is less benign than the primary procedure adds to the gravity of making an incorrect decision.
The ideal surgical patient should present with a long pain-free interval after primary surgery, typical radicular pain, clear signs of nerve root tension and compression, and a concordant finding of a recurrent disc prolapse on MRI scan. If there is any uncertainty, there should be a positive response to a nerve root injection.
While the general recommendation for a primary herniation is to wait six weeks before operating, this rule is less clear in the case of recurrent herniation. Spontaneous resolution is less likely in recurrent herniations, so if the diagnosis is clear and especially if there is a neurological deficit or significant pain, revision surgery should be considered earlier than six weeks.
The corollary is that the outcome of revision discectomy is inferior to that of primary surgery, and one should be wary of surgery in uncertain cases. In such cases, one should allow sufficient time to pass for the clinical picture to become stable and for reassessment and perhaps for reimaging to be undertaken.
Techniques
Revision discectomy
Revision discectomy is the mainstay of treatment for recurrent herniation. The surgical technique is covered in detail elsewhere in this publication.
Revision can be undertaken in many ways, as can primary discectomy. Broadly, these can be divided into conventional discectomy (most commonly microdiscectomy) and minimally invasive discectomy (most commonly endoscopic). Studies have shown the outcomes to be similar between these approaches,35 but with superior intraoperative measures including operation time and blood loss for minimally invasive techniques.36
Revision surgery is more challenging with distorted anatomical planes and perineural scarring, and this is reflected in the results. Most studies have found the outcome of revision discectomy to be inferior to that of primary discectomy in measures such as ODI, leg VAS and health status,20,37,38 while others have found minimal difference in clinical39 and patient-reported outcomes.40 There is an increased rate of dural tears ranging from to 4 to 6% compared to 1 to 2% in primary surgery,20,35 but there is not a clear difference in the rate of nerve injury.
Fusion
Because the limitations of revision discectomy include risk of re-recurrence, ongoing back pain and potential for instability from more aggressive facetectomy, some advocate adding a spinal fusion, usually using an interbody technique. In a recent review, no evidence was found to support the idea of routinely adding a fusion,35 with a similar rate of satisfactory clinical outcome for patients undergoing revision discectomy or fusion. However, patients undergoing fusion surgery reported a greater reduction in back pain. A randomized controlled trial comparing revision discectomy to fusion showed similar clinical results, but those undergoing discectomy had a higher rate of back pain, re-recurrence and dural tear.41 These results must be interpreted with the knowledge that fusion surgery is associated with a higher cost and complication rate when compared to revision discectomy.
For recurrent herniation, a fusion should be considered for i) the second or third recurrence or perhaps a very early recurrence, where the annulus is more likely to be incompetent, ii) the presence of significant back pain, as fusion is more likely to improve this, iii) incomplete pain relief after the primary discectomy, iv) signs of instability or significant degeneration on imaging, and v) requirement for removal of significant amount of facet joint to adequately access the herniation and nerve safely.
ILLUSTRATIVE CASE
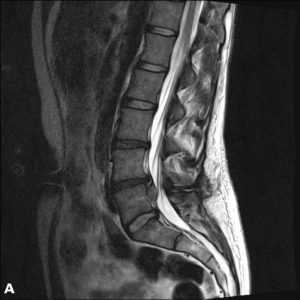
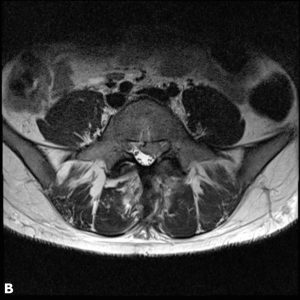
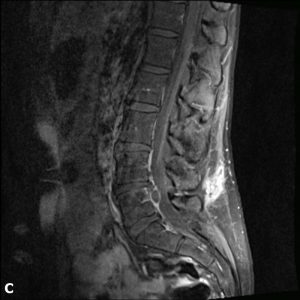
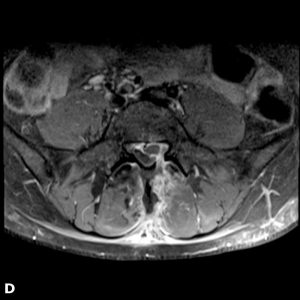
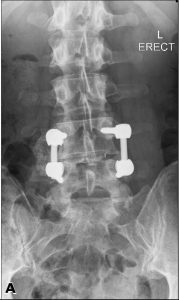
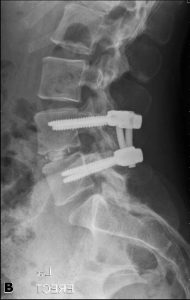
A 32-year-old female administrative worker underwent an uncomplicated microdiscectomy after six weeks of typical left L5 sciatica due to an L4-5 disc herniation. After a pain-free interval of four months, her symptoms returned. Her pain was somewhat different in that it did not radiate past the knee and was worsened by sitting. On examination, she still had mild weakness of great toe dorsiflexion but compared to before surgery, her SLR was less restricted and she had no ankle weakness. MRI showed a recurrent disc herniation with a sequestrated mass in the epidural space and with an enhancing rim on post-gadolinium fat-saturated T1 images (Fig. 2-2). She underwent revision discectomy, which was uncomplicated and significantly relieved her symptoms. However, pain returned within three months, and MRI showed another reherniation. It was decided to offer definitive surgery in the form of an interbody fusion (Fig. 2-3), which proceeded uneventfully and resulted in complete resolution of pain and a high level of patient satisfaction.
PEARLS AND PITFALLS
- Inform patients undergoing primary discectomy that there is a 5–10% risk of recurrence, which is greater if they are obese, and perhaps if they are diabetic or smoke.
- Fragmentectomy is better than aggressive discectomy for the primary surgery but may have a higher risk of recurrence.
- There is no need to restrict postoperative activity after primary or revision discectomy once the wound heals.
- Temper your enthusiasm for revision in cases with doubtful clinical features even if MRI shows a recurrence.
- Counsel the patient that the outcome of revision discectomy is not as good as that of primary discectomy and that the complication rate is higher, especially for a dural tear.
- Consider fusion in cases of second recurrence, especially if there is significant back pain or disc degeneration on imaging.
REFERENCES
- Huang W, Han Z, Liu J, Yu L, Yu X. Risk factors for recurrent lumbar disc herniation: a systematic review and meta-analysis. Medicine. 2016;95(2):e2378.
- Bohl DD, Ahn J, Mayo BC, et al. Does greater body mass index increase the risk for revision procedures following a single-level minimally invasive lumbar discectomy? Spine. 2016;41(9):816-821.
- Belykh E, Krutko AV, Baykov ES. Griers MB, Preul MC, Byvaltsev VA. Preoperative estimation of disc herniation recurrence after microdiscectomy: predictive value of a multivariate model based on radiographic parameters. Spine J. 2017;17(3):390-400. Epub 2016 Oct 17.
- Yao Y, Liu H, Zhang H, et al. Risk factors for recurrent herniation after percutaneous endoscopic lumbar discectomy. World Neurosurg. 2017;100:1-6.
- Meredith DS, Huang RC, Nguyen J, Lyman S. Obesity increases the risk of recurrent herniated nucleus pulposus after lumbar microdiscectomy. Spine J. 2010;10(7):575-580.
- Weinstein JN, Tosteson TD, Lurie JD, et al. Surgical vs nonoperative treatment for lumbar disk herniation: the Spine Patient Outcomes Research Trial (SPORT): a randomized trial. JAMA. 2006;296(20):2441-2450.
- Carragee EJ, Spinnickie AO, Alamin TF, Paragioudakis S. A prospective controlled study of limited versus subtotal posterior discectomy: short-term outcomes in patients with herniated lumbar intervertebral discs and large posterior anular defect. Spine. 2006;31(6):653-657.
- Licina P. Introduction of the Barricaid annular closure device - caution with new technology. Presented at: Spineweek 2016; May 16-20, 2016; Singapore. https://program.spineweek2016.com/proceedings. Accessed January 6, 2017.
- Caspar W, Campbell B, Barbier DD, Kretschmmer R, Gotfried Y. The Caspar microsurgical discectomy and comparison with a conventional standard lumbar disc procedure. Neurosurgery. January 1991;28(1):78-86.
- Williams RW. Microlumbar discectomy: a conservative approach to the virgin herniated lumbar disc. Spine. 1978;3(2):175-182.
- Shamji MF, Bains I, Yong E, Sutherland G, Hurlbert RJ. Treatment of herniated lumbar disk by sequestrectomy or conventional diskectomy. World Neurosurgery. 2014;82(5):879-883.
- Thomé C, Barth M, Scharf J, Schmiedek P. Outcome after lumbar sequestrectomy compared with microdiscectomy: a prospective randomized study. J Neurosurg Spine. 2005;2(3):271-278.
- Barth M, Diepers M, Weiss C, Thomé C. Two-year outcome after lumbar microdiscectomy versus microscopic sequestrectomy: part 2: radiographic evaluation and correlation with clinical outcome. Spine. 2008;33(3):273-279.
- Fakouri B, Shetty NR, White TC. Is sequestrectomy a viable alternative to microdiscectomy? A systematic review of the literature. Clin Orthop Relat Res. 2015;473(6):1957-1962.
- Ran J, Hu Y, Zheng Z, et al. Comparison of discectomy versus sequestrectomy in lumbar disc herniation: a meta-analysis of comparative studies. PLoS One. 2015;10(3):e0121816.
- Ellenbogen JR, Marlow W, Fischer BE, Tsegaye M, Wilby MJ. Is the rate of re-operation after primary lumbar microdiscectomy affected by surgeon grade or intra-operative lavage of the disc space? Br J Neurosurg. 2014;28(2);247-251. Epub 2013 Aug 19.
- Carragee EJ, Helms E, OʼSullivan GS. Are postoperative activity restrictions necessary after posterior lumbar discectomy? A prospective study of outcomes in 50 consecutive cases. Spine. 1996;21(16):1893-1897.
- Newsome RJ, May S, Chiverton N, Cole AA. A prospective, randomised trial of immediate exercise following lumbar microdiscectomy: a preliminary study. Physiotherapy. 2009;95(4):273-279.
- Licina P. Accelerated patient guided return to activity after lumbar discectomy is safe. Presented at: Australian Orthopaedic Association Annual Scientific Meeting 2015; October 11-15, 2015; Brisbane, Australia. https://www.aoa.org.au/eproceedings/eproceedings/eproceedings-presentation?pid=1345. Accessed January 6, 2017.
- Palma L, Carangelo B, Muzii VF, Mariottini A, Zalaffi A, Capitani S. Microsurgery for recurrent lumbar disk herniation at the same level and side: do patients fare worse? Experience with 95 consecutive cases. Surg Neurol. 2008;70(6):619-621.
- Parker SL, Mendenhall SK, Godil SS, et al. Incidence of low back pain after lumbar discectomy for herniated disc and its effect on patient-reported outcomes. Clin Orthop Relat Res. 2015;473(6):1988-1999.
- Lebow RL, Adogwa O, Parker SL, Sharma A, Cheng J, McGirt MJ. Asymptomatic same-site recurrent disc herniation after lumbar discectomy: results of a prospective longitudinal study with 2-year serial imaging. Spine. 2011;36(25):2147-2151.
- Annertz M, Jönsson B, Strömqvist B, Holtås S. Serial MRI in the early postoperative period after lumbar discectomy. Neuroradiology. 1995;37(3):177-182.
- Floris R, Spallone A, Aref TY, et al. Early postoperative MRI findings following surgery for herniated lumbar disc. Acta Neurochir (Wien). 1997;139(3):169-175.
- Heindel P, Tuchman A, Hsieh PC, et al. Reoperation rates after single-level lumbar discectomy. Spine. 2017;42(8):E496-E501.
- Lisle DA. Imaging for Students. 4th ed. London: Hodder Education; 2012.
- van de Kelft EJ, van Goethem JW, de La Porte C, Verlooy JS. Early postoperative gadolinium-dTPA-enhanced MR imaging after successful lumbar discectomy. Br J Neurosurg. 1996;10(1):41-49.
- Deutsch AL, Howard M, Dawson EG, et al. Lumbar spine following successful surgical discectomy. Spine. 1993;18(8):1054-1060.
- Babar S, Saifuddin A. MRI of the post-discectomy lumbar spine. Clin Radiol. 2002;57(11):969-981.
- Barrera MC, Alustiza JM, Gervas C, Recondo JA, Villanua JA, Salvador E. Post-operative lumbar spine: comparative study of TSE T2 and turbo-FLAIR sequence vs contrast-enhanced SE T1. Clin Radiol. 2001;56(2):133-137.
- Guterl CC, See EY, Blanquer SB, et al. Challenges and strategies in the repair of ruptured annulus fibrosus. Eur Cell Mater. 2013;25:1-21.
- Hahne AJ, Ford JJ, McMeeken JM. Conservative management of lumbar disc herniation with associated radiculopathy: a systematic review. Spine. 2010;35(11):E488-E504.
- Manchikanti L, Benyamin RM, Falco FJ, Kaye AD, Hirsch JA. Do epidural injections provide short- and long-term relief for lumbar disc herniation? A systematic review. Clin Orthop Relat Res. 2015;473(6):1940-1956.
- Karamouzian S, Ebrahimi-Nejad A, Shahsavarani S, Keikhosravi E, Shahba M, Ebrahimi F. Comparison of two methods of epidural steroid injection in the treatment of recurrent lumbar disc herniation. Asian Spine J. 2014;8(5):646-652.
- Dower A, Chatterji R, Swart A, Winder MJ. Surgical management of recurrent lumbar disc herniation and the role of fusion. J Clin Neurosci. 2016;23:44-50.
- Li X, Hu Z, Cui J, et al. Percutaneous endoscopic lumbar discectomy for recurrent lumbar disc herniation. Int J Surg. 2016;27:8-16.
- Buchmann N, Preuß A, Gempt J, et al. Outcome after surgical treatment for late recurrent lumbar disc herniations in standard open microsurgery. World Neurosurg. 2016;89:382-386.
- Lubelski D, Senol N, Silverstein MP, et al. Quality of life outcomes after revision lumbar discectomy. J Neurosurg Spine. 2015;22(2):173-178. Epub 2014 Dec 5.
- Yoshihara H, Chatterjee D, Paulino CB, Errico TJ. Revision surgery for “real” recurrent lumbar disk herniation: a systematic review. Clin Spine Surg. 2016;29(3):111-118.
- Papadopoulos EC, Girardi FP, Sandhu HS, et al. Outcome of revision discectomies following recurrent lumbar disc herniation. Spine. 2006;31(13):1473-1476.
- El Shazly AA, El Wardany MA, Morsi AM. Recurrent lumbar disc herniation: a prospective comparative study of three surgical management procedures. Asian J Neurosurg. 2013;8(3):139-146.