Gill Dickson and Suzanne M. McDonough
INTRODUCTION
Low back pain is a global problem that is highly prevalent in the general population, frequently episodic and persistent. Many will resolve their spinal pain with simple measures, including simple analgesia, therapy and exercise advice. However, the major part of the cost of spinal pain to the National Health Service (NHS) in the UK, estimated to be £12.3 billion annually,1 is from the proportion of persons with spinal pain whose symptoms become chronic. Research has suggested that the longer an individual is disabled by spinal pain, the less chance he or she has of returning to work, and the more health care he or she will require.
A potential explanation of the healthcare costs associated with spinal pain is the overall passive nature of the intervention; low back pain frequently recurs, and patients return for repeated passive treatment. A potential solution is for patients to have active involvement in their own health care, using self-management to decrease this burden.2
DEFINITION OF SELF-MANAGEMENT
There are a multitude of definitions for self-management in the literature. Taylor et al.3 used the definition by the US Institute of Medicine,4 “The tasks that individuals must undertake to live with one or more chronic conditions. These tasks include having the confidence to deal with medical management, role management and emotional management of their conditions.”
Taylor et al.5 identified what a self-management support program might include and emphasized the need for the person to be an active participant in the process, “Self-management education programmes are distinct from simple patient education or skills training, in that they are designed to allow people with chronic conditions to take an active part in the management of their own conditions.”
Others have provided a conceptual definition of self-management6 as a structured multicomponent intervention that supports autonomy and involves education and training with the aim of promoting adherence to self-management behaviors, such as self-regulation, physical activity and pain management, to achieve improved physical, psychological and economic outcomes. This definition is helpful in that it not only makes it clear that for self-management to work the patient needs to take ownership, with assistance from the therapist, but specifies some of the self-management behaviors that need to be in place for this to happen, e.g., exercise, pain coping skills, problem solving, decision making, communication and goal setting. It is important for the patient to be ready to take action and for the therapist to form a relationship with the patient that supports autonomy, so avoiding a paternalistic relationship.
Although, in the section below, we present each component of self-management separately, it is worth noting that in a recent rapid systematic review no one component in the largely multicomponent interventions stood out as more important than any other, and the two most common components of self-management support interventions were education and psychological support.3 Two other systematic reviews also inform this area.5,6
THE VALUE OF SELF-MANAGEMENT IN LOW BACK PAIN
Supporting patients to be autonomous by giving patient’s ownership of their own health condition and being aware of how to reduce, prevent and manage symptoms, health care professionals feel they are empowering patients by giving them tools to change. However, the evidence2 shows moderate quality evidence of only small effects of self-management programs on pain and disability in people with low back pain. These relatively small effects may be partly explained by the fact that in practice there is evidence of a gap between therapists approach to self-management strategies and the implementation of these strategies by patients to change their behavior. In the past there has been an assumption that for those patients with chronic or long-term conditions providing education and advice should facilitate self-management, yet high levels of non-adherence to clinical advice have been reported.7
Self-management does not mean leaving patients to manage their health condition without support. Instead, self-management means equipping patients with the right tools to understand their health condition and through empowerment transferring from a passive “fix me” approach to being in control. Health professionals have a vital part to play in supporting patients to self-manage. In order for self-management to be implemented into clinical practice, a whole systems approach is needed that depends on the organization to ensure that patients receive appropriate self-management programs (e.g., multicomponent programs) and that the professional receives training in behavior change strategies, material resources and has time to implement the self-management program as part of care for the patient.3 Historically, health care, including physiotherapy, has rarely been based on relevant behavior change theory, which could explain the lack of adherence by patients.7 There are many strategies that can support low back pain patients with self-management. These strategies need to be embedded within interventions designed to promote behavior change, in particular identifying whether the patient is ready to become autonomous and what would assist them to become “ready to change.” Burd and Hallsworth review tools to assist practitioners to move people to a place where they are ready to change.8
TIMING OF SELF-MANAGEMENT
The 5 Year Forward View9 lays out a clear direction for the NHS to lead us to a better future in terms of health. There has been a call for a radical upgrade in prevention and public health in order to reduce preventable, chronic/long-term conditions so that the NHS will be sustainable. However, it is important to note that self-management tools need to be viewed in all aspects of back care management and not solely for chronic long-term conditions. Thus, low back pain management in all aspects of the care pathway, including early self-management, is endorsed in the most recent NICE guidelines.10 The Start Back trial was published in the Lancet in 201111 and looks at both clinical and cost effectiveness of a stratified management approach, allocating patients to different treatment pathways based on their prognosis (low, medium or high risk of poor outcome) with current best practice. The use of screening tools such as the STarT Back (SBST) can support clinicians in identifying categories of risk of poor outcome and, thereby, selecting the appropriate patients for intervention. Using this tool the low risk patients who would be identified are recommended to seek activity and self-management is encouraged.
SELF-MANAGEMENT STRATEGIES FOR LOW BACK PAIN
The recent NICE guidelines10 recommend that self-management is an integral part of low back pain management. This includes providing people with advice and information, tailored to their needs and capabilities, to help them self-manage their low back pain with or without sciatica, at all steps of the treatment pathway. It includes giving information on the nature of low back pain and sciatica, and encouragement to continue with normal activities.
Lifestyle Advice/Health Promotion
In the United Kingdom and other Western countries, we eat to excess, drink to excess, forgo exercise, and work long hours, often under an incredible degree of stress and pressure. These modifiable lifestyle factors are important as many chronic/long-term diseases share common behavioral risk factors, including inactivity, alcohol consumption, smoking and an unhealthy diet; all of which are well documented as risk factors for low back pain. Associations have been found between lumbar radicular pain in smokers, patients who are overweight, and patients with high levels of physical activity. A sedentary lifestyle/lack of exercise leads to weakness of supporting muscles and ligaments, which is also known to contribute to spinal pain. It is an important that these factors are addressed by health professionals in the self-management of spinal pain.
Evidence in the literature suggests that smoking has a detrimental effect on the spine. A large robust US study of almost 35,000 participants demonstrated a higher proportion of back pain in smokers than non-smokers and a higher prevalence of back pain amongst those who smoke more cigarettes.12 Patients with back pain do not, however, necessarily link their spinal problem with smoking. Brady et al.13 carried out a questionnaire study on 10,000 women at time periods over 12 years to look at the relationship between weight, physical activity and back pain in young women. Higher weight, age, inadequate levels of physical activity and depression were all found to be independent predictors for back pain.
Stress does affect everyone; however, high stress levels are known to have a detrimental effect on physical health. Busyness and stress limit free and available time to exercise and sleep; eating habits are also affected as well as posture. Stress is known to increase muscle tension, causing additional tightness, restriction and pressure on the spine.
From a clinical perspective, education about lifestyle factors and an exercise plan worked through by the patient are considered to go a long way towards resolving these lifestyle related problems. There is excellent guidance on how a clinician can provide a very brief intervention to address lifestyle factors during a consultation. Indeed, a framework which includes training for staff in delivering this very brief advice has been developed in the UK and is called “Making every contact count or MECC.”14 MECC is a very brief intervention (30 seconds to 3 minutes) that involves using every opportunity to promote health and well-being as a means of achieving long term behavior change.This approach uses the millions of day-to-day interactions that organizations and individuals have with the public to support them in making positive changes to their physical and mental health and well-being. The NHS recommends that every encounter should be seen as opportunity to engage in MECC in order to promote health and wellness.
However, the supporting evidence for including lifestyle advice is less clear. For example, in a recent systematic review Taylor et al.5 attempted to explore the effect of including a lifestyle component in self-management interventions for chronic pain and showed no difference between those with and without a lifestyle component. However, they concluded that this analysis was exploratory and tentative. With respect to education, there was inconclusive positive evidence. However, education may be more effective when delivered in an active format that promotes participation, rather than a passive process.3
Exercise
The World Health Organization has a global goal to promote and protect health through healthy eating and physical activity. Physiotherapy is helping to meet this goal; as the provision of one form of physical activity, a structured exercise program for patients with low back pain is a routine part of a physiotherapy consultation. In addition advice and information leaflets have gone some way to promoting exercise as a self-management strategy outside of the consultation in order to empower patients to promote behavior changes. There is no doubt that exercise is beneficial for patients with low back pain and the tailoring of this to the individual is a key part of the health professional role. A recent systematic review to determine which exercise interventions are the most effective at reducing low back pain (n=39 trials) has shown that exercise leads to greater improvements in strength, resistance and coordination/stabilization when compared to a control group.15 There has been increasing interest in comparing the effects of specific exercise for low back pain with more general “physical activity” for low back pain. The results of these demonstrate similar long term outcomes although there is some evidence to suggest greater improvement in pain in the short term for patients with stability exercises. For example, there appears to be evidence in favor of interventions with a physical activity component (e.g., any exercise, yoga, Tai Chi, posture5) and more specifically walking for non-specific low back pain,16,17 which has shown similar effects to supervised group-based exercise classes (based on back to fitness) or standard physiotherapy.18 Ongoing research will help inform this debate for lumbar stenosis; the BOOST trial, studying the physiotherapy treatment of back and leg pain or symptoms due to lumbar stenosis, is currently underway in the UK. Using 12 UK sites, it aims to compare specific individual exercises and management to general activation in patients over 65.19
One frequently encountered challenge in using exercise or physical activity as part of rehabilitation is the proportion of patients who do not actively engage in the prescribed home exercise or physical activity program. Physiotherapists need to understand the complex factors contributing to the adherence to exercise in order to tailor and support self-management more effectively. Beinart et al.,20 with a systematic review, looked at identification of these factors in adults with chronic low back pain. They found that greater health locus of control, supervision and participation in a general behavior change program that incorporates motivational strategies all increased patient adherence to a prescribed exercise program. Using behavior change strategies, such as motivational interviewing, is known to produce better outcomes than physiotherapy alone in people with chronic low back pain.21
Psychological Strategies
The importance of psychological support in spinal pain emerges from a body of qualitative and quantitative evidence.3,5 The qualitative synthesis discusses the difference in expectations between the patient and the healthcare professional, with the patient initially seeking a “cure” for their pain. Psychological support is highlighted as a means of assisting individuals in the adjustment process as they begin to manage their expectations more realistically. This evidence states that this is most helpful in the initial stages of spinal pain, whereas some patients with longer-standing pain tend to have more realistic expectations, which are more congruent with those held by healthcare professionals. Many of the strategies used to provide psychological support are combined in interventions, and the quantitative evidence supports the use of a range of strategies such as fear avoidance, coping skills, goal setting/action planning, modeling by others, problem solving, pain reconceptualization, attention distraction and graded exposure. There is also support for different psychological approaches such as cognitive behavioral therapy or operant conditioning,5 although it is worth noting that cognitive behavioral therapy is supported in the most recent NICE guidelines.22
Education and Challenging Beliefs
A key part of self-management in spinal pain is to educate the patient and so help them understand their back pain and challenge negative beliefs. Although the effect of education appears to be positive, it is important to take people’s previous educational experiences into account as they may feel intimidated by the approach used, and this can reduce their confidence in their ability to self-manage their back pain. For example, in a recent systematic review,5 although there was some evidence in favor of a medical education component with regard to anxiety in the short term and pain intensity and depression in the medium to long term, inclusion of medical education was associated with lower self-efficacy. Perhaps this effect on self-efficacy can be explained by past negative educational experiences, such that the discussion part of education sessions on self-management programs are intimidating, especially when individuals are required to give feedback on their goal-setting exercises.5
In terms of approaches to health education, systematic reviews have supported the benefits of the use of the Health Belief Model.23 The Health Belief Model theorizes that, in order for behavior change to take place, the individual must first believe that change is both possible and beneficial. For patients with low back pain, the concepts concern beliefs regarding susceptibility to the development of symptoms and the potential consequences. Behavioral evaluation then consists of the beliefs of performing recommended health behaviors and the barriers to changing symptom related behaviors. The Health Belief Model also suggests that behavior is influenced by cues to action. These can include circumstances, events, people and things that motivate behavior change.
Sharafkhani et al.23 carried out a quasi-experimental study to look at the effect of an educational intervention program on the adoption of low back pain preventative behaviors using this Health Belief Model approach with nurses. The results showed that an educational intervention program based on the Health Belief Model could promote preventative behaviors within this group. Other studies used this approach as a self-management approach for various health conditions. For example, Sadeghi et al.24 looked at a Health Belief Model as a self-management tool within a chronic dermatology condition. The results of this study showed the positive effects of this model-based educational program as a tertiary preventive measure on adopting self-care behaviors in patients that can help them achieve self-efficacy in controlling their disease and enhancing their treatment process.
Challenging beliefs through patient-centered communication used to enhance motivation and change behavior is a key to self-management. Evidence suggests that fear avoidance beliefs are associated with poor treatment outcomes in patients with low back pain of less than six months, and thus, early treatment, including interventions to reduce fear, may avoid delayed recovery and chronicity. Patients with high fear avoidance beliefs are more likely to improve when these are addressed in treatments than when fear avoidance beliefs are present.25 By addressing beliefs and challenging them to change, these improvements are realized.
Shared Decision Making
The NHS in the UK introduced the RightCare Shared Decision Making program in 2012 to promote patient-centered care and encourage patients to be actively involved in healthcare decisions and take ownership of their health.26 It is a process in which patients, when they reach a decision crossroads in their health care, can review all the treatment options available to them and participate actively with their healthcare professional in making that decision.
The importance of shared decision making emerged as a key issue in a meta-analysis of qualitative and quantitative reviews of self-management in long term conditions including pain.3 Individuals should be actively involved in the decision-making processes aiming to increase independence and facilitate self-management. However, self-management interventions, where patients are left to manage their own condition with minimal oversight or active involvement of the health-care provider, showed small effects on pain and disability in people with low back pain.3 This highlights the importance of active involvement of the health care provider as part of the process.
Patient’s Story
Sarah (not the patient’s real name) is a 64-year-old patient with degenerative arthritis in both knees. She had suffered problems with her knees for many years and was first prescribed anti-inflammatory and pain relief medication 11 years ago, but she felt unable to pursue other treatments while working full time. “I’ve worked for 49 years, but always said that when I retired, I would take a step forward and start doing something else about my knees.” Sarah did just that when she retired last year, but the prospect of knee replacement surgery was a real worry to her. She was referred to the musculoskeletal (MSK) service and initially assessed by an Advanced Musculoskeletal Practitioner, specializing in lower limbs. The clinician assessed Sarah’s situation and discussed her treatment options using an option grid. Sarah describes the experience:
“Surgery is the bottom line for me, but knee replacements are not a route I’m prepared to go down at the moment, I’m 110% wimp! The clinician discussed alternatives to surgery with me using the option grid and gave me lots more information about the different options to take away and read. The clinician was brilliant; she couldn’t have been more helpful if she tried.
The option grid was really useful, you read a lot about different ways of managing your condition in the papers and elsewhere and wonder if they are really a good idea. But receiving information directly from a health professional, who talked the options through with me, finalized it for me and I decided to have the steroid injection to help make me more mobile.”
Sarah, now receiving physiotherapy, has been given exercises to help her knees and is considering acupuncture therapy.
Information
Patients require access to quality, evidenced-based information so that they can take part in decisions about their health care. It is crucial that these resources provide information about the condition and encourage prompt activation and improve knowledge. The Chartered Society of Physiotherapy27 myth buster campaign of 2016 has been widely used to educate patients and equip them with the knowledge to understand their condition. There is evidence that information combined with exercise reduces chronicity.
Access to appropriate information to ensure that patients are empowered to make the right choices is crucial. The use of the voluntary and third sector organizations, such as lifestyle hubs, is crucial support. The emphasis now is on normalizing and restoring activity levels to facilitate function and reduce chronicity. Taking the exercise and lifestyle support into the community and out of health care setting de-medicalizes the condition and supports the aim to reduce chronicity.
Telehealth
Telehealth includes the use of apps, web, and text reminders. These modalities are available to us to provide support to enable patients with low back pain to self-manage with confidence. There were 42.4 million smartphone users in the UK during 2016; this number is expected to rise to 64 million by 2018. The use of apps in management of health conditions has grown significantly since the rise of smartphones. The rise in technology and IT means that we can get readily available advice and education at the click of a button. This is the method we use to fix something at home and the first thing we do if we want to research a condition further. We have an essential role as a guide in this; we need to ensure that patients are accessing the right information to support them with their condition.
The creation and use of apps, information available on the Internet and NICE guidance are leading to a cultural power shift. Patients are able to take ownership of their health condition via online support groups and access to information and advice.
De Jongh et al.28 carried out a Cochrane database systematic review that looked at mobile phone messaging for facilitating self-management of long-term illnesses. They found some, albeit very limited, indications that in certain cases mobile phone messaging interventions may support the self-management of long-term illnesses. However, the review demonstrated that there are significant information gaps regarding the long-term effects, acceptability, costs and risks of such interventions. This review highlights that further research into these issues is needed.
PhysioDirect
Initiated as a result of long delays in accessing physiotherapy for musculoskeletal problems, several areas in the UK have introduced PhysioDirect services in which patients telephone a physiotherapist for initial assessment and treatment advice without waiting for a face-to-face appointment. Patients can be given advice about self-management and exercises, as well as the need and priority for seeing a health care professional face-to-face. A large National Institute of Health Research (NIHR) funded trial has shown that providing physiotherapy via PhysioDirect is equally clinically effective compared with usual waiting list-based care, provides faster access to treatment, appears to be safe and is broadly acceptable to patients. PhysioDirect is probably cost-effective compared with usual care.29
One benefit of a hands-off, telephone assessment and advice program is that patients are supported to self-manage, preventing a passive, “fix me” mentality. Through this approach clinicians are best placed to provide patients with active strategies to support recovery. In practice, traditional physiotherapy assessments rely on both verbal and non-verbal cues to determine a clinical impression and inform a management plan. Clinicians carrying out these telephone assessments, therefore, need to be experienced in clinical assessments and remain vigilant for red flags and yellow flags. Within clinical practice, an option of a face-to-face appointment for any failure to improve and a follow-up telephone review are some of the safety nets that can be implemented to mitigate this.
The progression of IT—telehealth, apps, and electronic exercise and advice packages—can be used to support PhysioDirect as an assessment and management plan.
Professional Support
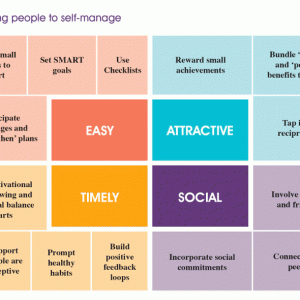
As mentioned earlier self-management strategies need to be underpinned by behavior change theory. The importance of behavior change is highlighted by a recent guide released by NHS England as part of the funded “Realising the Value” program, which seeks to develop person- and community-centered approaches for health and well-being. The guide offers two things: a framework for understanding and changing behavior and real-world examples of how these changes happen in practice. It is written for people who support those living with long-term conditions, or who help people avoid these conditions using person- and community-centered approaches.8 This guide helps to explain why it is so challenging for people to self-manage their health, e.g., “People tend to be confronted with much more information than they are willing or able to process; people seek to minimize effort and are disproportionately affected by small barriers to change; people typically stick with the way things are—the status quo; people tend to interpret facts using mental “shortcuts” (rules of thumb or assumptions) that confirm existing views.”8 The authors of the report have developed a framework called EAST which they consider to be an accessible way of applying behavior change theory in practice. The core message of EAST is that, if you want to encourage a behavior, you should make it Easy, Attractive, Social and Timely8 (Fig. 3-1).
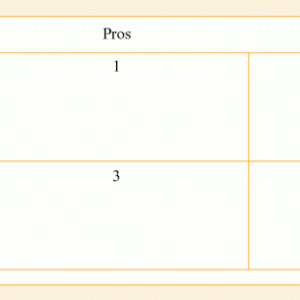
As mentioned earlier this guide gives examples of tools that can assist with moving people to a stage where they are ready to change.8 Figure 3-2 is an example of a decisional balance chart that can be used to hold a conversation about a behavior that a person may want to change and spark their motivation to change. The authors of this guide highlight the need for careful handling of this tool, as it is possible that encouraging someone to contemplate the pros of their current behavior may reinforce the behavior. They recommend that practitioners are trained in motivational interviewing and include a link to recognized courses.
Another initiative within the NHS to assist practitioners to support patients to change their behavior, mentioned earlier in this chapter, is MECC.14 The website is a useful resource and links to NICE “Behaviour Change Guidance - Individual Approaches”30 (as well as e-learning on MECC).31 Very brief advice is recommended in the NICE22 behavior change guidance.
Other initiatives have recognized that in order for clinicians to promote health they need to have the skills to embed behavior change techniques within their practice, and there is some evidence that training to improve healthcare practitioners’ communication behaviors can assist them to more fully support their patients’ efforts to change their behavior.7 One approach to training is based on self-determination theory which states that in order for people to change their behavior (e.g., adhere to advice or participate in exercise), people need to feel that they have choice over their behavior (or have autonomy), that they are capable (e.g., capable of change), and that they belong in a social group (e.g., have opportunity to change). Using this approach the therapist considers the perspective of the patient, provides relevant information and opportunities for choice, and encourages the individual to accept personal responsibility for health behaviors without judging or coercing the patient. In contrast, a controlling health care climate involves disregarding patients’ views, pressuring patients and making the decisions on the patients’ behalf without consultation. Unfortunately, research has indicated that when interacting with patients, physiotherapists and other healthcare practitioners often adopt a controlling approach.7
Organization Strategy
Access to self-management resources (timing and mode of access)
Many people build health-promoting habits into their lives self-sufficiently. For those who are ready to start self-managing, encountering difficulties when seeking out support can mean that they do not even get started. Barriers can include: needing to be referred into a service before accessing it; not knowing how to get to the location where support is provided; requiring people to fill out forms or undertake other activities before accessing support; or not making a specific plan to access support on the day it is scheduled.8 There are various ways that healthcare and community-based providers can support patients on this journey. The ability to gain direct access to services, including self-referral to physiotherapy, enables early intervention and self-management support. More recently the use of MSK physiotherapists as first point of triage in primary care are showing some promising results, supporting early self-management, appropriate signposting and reducing GP appointment times.
CONCLUSION (PEARLS AND PITFALLS)
Self-management of spinal pain requires us to consider medical health management, patient roles and social needs, and psychological factors. As health practitioners we need to ensure that the information given on a condition is clear, accurate and accessible in different information formats, including though the use of technology. The roles of the patient in society, including occupation, social situation and lifestyle factors, all need to be considered. Patients need to understand the benefits and pitfalls of different lifestyle choices in relation to their spinal pain condition, with information readily on hand, and access to services as required, including the voluntary sector, to support them in making appropriate lifestyle changes. In order to be successful in implementing changes, there needs to be a willingness to make the change on the behalf of the patient, and the clinicians need to have the appropriate skills to assist the patient to change their behavior. For example the clinician needs to be able to challenge beliefs and initial expectations, using behavior change strategies and psychological strategies, such as cognitive behavioral therapy. Some steps have been made towards this goal; however, health professionals and community partnerships need to provide a consistent message and work together to empower those with spinal pain. This will help patients understand their spinal pain, what to expect, what to do and their vital role in how to live, which will go a long way towards determining the future outcome of their condition.
SUGGESTED READING
- Cooper K, Smith B, Hancock E. Patients’ perceptions of self-management of chronic low back pain: evidence for enhancing patient education and support. Physiotherapy. 2009;95(1):43-50.
- Foster G, Taylor SJC, Eldridge SE, Ramsay J, Griffiths CJ. Self-management education programmes by lay leaders for people with chronic conditions. Cochrane Database Syst Rev. 2007;(4):CD005108.
- Hurley DA, Murphy LC, Hayes D, et al. Using intervention mapping to develop a theory-driven, group-based complex intervention to support self-management of osteoarthritis and low back pain (SOLAS). Implement Sci. 2016;11:56.
- LeFort S, Gray-Donald K, Rowat KM, Jeans ME. Randomized controlled trial of a community-based psychoeducation program for the self-management of chronic pain. Pain. 1998;74(2-3):297-306.
- Linton SJ, McCracken LM, Vlaeyen JW. Reassurance: help or hinder in the treatment of pain. Pain. 2008;134(1-2):5-8.
- Williams A, Wiggers J, O’Brien KM, et al. A randomised controlled trial of a lifestyle behavioural intervention for patients with low back pain, who are overweight or obese: study protocol. BMC Musculoskeletal Disord. 2016;17:70.
REFERENCES
- Maniadakis N, Gray A. The economic burden of back pain in the UK. Pain. 2000; 84:95-103.
- Oliveira VC, Ferreira PH, Maher CG, Pinto RZ, Refshauge KM, Ferreira ML. Effectiveness of self-management of low back pain: systematic review with meta-analysis. Arthritis Care Res (Hoboken). 2012;64(11):1739-1748.
- Taylor SJC, Pinnock H, Epiphaniou E, et al. A rapid synthesis of the evidence on interventions supporting self-management for people with long-term conditions: PRISMS – Practical systematic review of self-management support for long-term conditions. Southampton (UK): NIHR Journals Library; 2014.
- Adams K, Greiner AC, Corrigan JM, eds. The 1st Annual Crossing the Quality Chasm Summit – A Focus on Communities. Washington, DC: The National Academic Press; 2004.
- Taylor SJC, Carnes D, Homer K, et al. Improving the self-management of chronic pain: COping with persistent Pain, Effectiveness Research in Self-management (COPERS). Southampton (UK): NIHR Journals Library; 2016.
- Toomey E, Currie-Murphy L, Matthews J, Hurley DA. The effectiveness of physiotherapist-delivered group education and exercise interventions to promote self-management for people with osteoarthritis and chronic low back pain: a rapid review part I. Man Ther. 2015;20(2):265-286.
- Lonsdale C, Hall AM, Murray A, et al. Communication skills training for practitioners to increase patient adherence to home-based rehabilitation for chronic low back pain: results of a cluster randomized controlled trial. Arch Phys Med Rehabil. 2017;98(9):1732-1743.
- Burd H, Hallsworth M. Supporting self-management: a guide to enabling behaviour change for health and wellbeing using person- and community-centred approaches. 2016; https://www.health.org.uk/sites/health/files/RtVSupportingSelfManagement.pdf. Accessed July 2017.
- National Health Service (NHS). Five year forward view. NHS England. 2014; https://www.england.nhs.uk/wp-content/uploads/2014/10/5yfv-web.pdf. Accessed February 7, 2017.
- National Institute for Health and Care Excellence (NICE). Low back pain and sciatica in over 16s. NG59. London: NICE. 2016; https://www.nice.org.uk/guidance/ng59. Accessed June 11, 2018.
- Hill JC, Whitehurst DG, Lewis M, et al. Comparison of stratified primary care management for low back pain with current best practice (STarT Back): a randomised controlled trial. Lancet. 2011; 378(9802):1560-1571.
- Green BN, Johnson CD, Snodgrass J, Smith M, Dunn AS. Association between smoking and back pain in a cross section of adult Americans. Cureus. 2016;8(9):e806.
- Brady SR, Hussain SM, Brown WJ, et al. Relationships between weight, physical activity and back pain in young adult women. Medicine (Baltimore). 2016;95(19):e3368.
- National Health Service (NHS). Making Every Contact Count (MECC). Leeds, UK:Health Education England. 2018; http://www.makingeverycontactcount.co.uk/. Accessed July 18, 2018.
- Searle A, Spink M, Ho A, Chuter V. Exercise interventions for the treatment of chronic low back pain: a systematic review and meta-analysis of randomised controlled trials. Clin Rehabil. 2015;29(12):1155-1167.
- McDonough SM, Tully MA, Boyd A, et al. Pedometer-driven walking for chronic low back pain: a feasibility randomised controlled trial. Clin J Pain. 2013
- O'Connor SR, Tully MA, Ryan B, et al. Walking exercise for chronic musculoskeletal pain: systematic review and meta-analysis. Arch Phys Med Rehabil. 2015;96(4):724-734.
- Hurley DA, Tully MA, Lonsdale C, et al. Supervised walking in comparison with fitness training for chronic back pain in physiotherapy: results of the SWIFT single-blinded randomized controlled trial (ISRCTN17592092). Pain. 2015 Jan;156(1):131-147.
- Nuffield Department of Orthopaedics, Rheumatology and Musculoskeletal Sciences (NDORMS). BOOST: Better Outcomes for Older People with Spine Trouble. Oxford, UK: University of Oxford, Medical Sciences Division. 2018; https://www.ndorms.ox.ac.uk/clinical-trials/current-trials-and-studies/boost. Accessed August 22, 2018.
- Beinart NA, Goodchild CE, Weinman JA, Ayis S, Godfrey EL. Individual and intervention related factors associated with adherence to home exercise in chronic low back pain: a systematic review. Spine J. 2013;13(12):1940-1950.
- Vong SK, Cheing GL, Chan F, So EM, Chan CC. Motivational enhancement therapy in addition to physical therapy improves motivational factors and treatment outcomes in people with low back pain: a randomised controlled trial. Arch Phys Med Rehabil. 2011;92:176-183.
- National Institute for Health and Care Excellence (NICE). Behaviour change: individual approaches. PH49. London: NICE. 2014; https://www.nice.org.uk/guidance/ph49. Accessed June 10, 2018.
- Sharafkhani N, Khorsandi M, Shamsi M, Ranjbaran M. The effect of an educational intervention program on the adoption of low back pain preventive behaviors in nurses: an application of the health belief model. Global Spine J. 2016;6(1):29-34.
- Sadeghi R, Tol A, Moradi A, Baikpour M, Hossaini M. The impacts of a health belief model-based educational program on adopting self-care behaviors in pemphigus vulgaris patients. J Educ Health Promot. 2015;4:105.
- Wertli MM, Rasmussen-Barr E, Held U, Weiser S, Bachmann LM, Brunner F. Fear-avoidance belief–a moderator of treatment efficacy in patients with low back pain: a systematic review. Spine J. 2014;14(11):2658-2678.
- NHS Right Care. Right Decision Making Programme. Leeds, UK:NHS England. 2017; https://www.england.nhs.uk/rightcare/shared-decision-making. Accessed July 18, 2018.
- Chartered Society of Physiotherapy (CSP). Back pain myth busters. London, UK:CSP. 2016; https://www.csp.org.uk/public-patient/back-pain-myth-busters. Accessed August 22, 2018.
- De Jongh T, Gurol-Urganci I, Vodopivec-Jamsek V, Car J, Atun R. Mobile phone messaging for facilitating self-management of long-term illnesses. Cochrane Database Syst Rev. 2012;12:CD007459.
- Salisbury C, Foster NE, Hopper C, et al. A pragmatic randomised controlled trial of the effectiveness and cost-effectiveness of ‘PhysioDirect’ telephone assessment and advice services for physiotherapy. Health Technol Assess.2013;17(2):1-157.
- National Institute for Health and Care Excellence (NICE). Behaviour change: individual approaches. PH49. London: NICE. 2014: http://www.makingeverycontactcount.co.uk/media/1020/01_nice-behaviour-change-individual-approaches.pdf. Accessed August 22, 2018.
- National Health Service (NHS). Making Every Contact Count: E-Learning. Leeds, UK:Health Education England. 2018; http://www.makingeverycontactcount.co.uk/training/e-learning/. Accessed August 22, 2018.