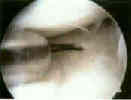
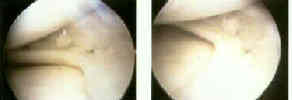
- Meniscal Anatomy and Physiology:
- medial meniscus
- bucket handle meniscus tear
- posterior horn tears of medial meniscus
- lateral meniscus
- discoid meniscus
- indications for repair:
- any peripheral nondegenerative longitudinal tears < 3 cm;
- if tear is w/in 3 mm of the periphery, it is considered vascular;
- area 3-5 mm from periphery is grey zone, & > 5 mm from periphery is considered avascular;
(see vascularity of the meniscus)
- unstable tears or tears within vascular zone that are > 7 mm are repairable;
- mobile, single, vertical, longitudinal tear of the meniscus limited to vascular outer one-third of the meniscal substance;
- relative contra-indications:
- tears greater than 3 cm do not seem to heal, following surgery;
- transverse tears, even in the periphery, do not seem to heal;
- do not repair flap tears, radial tears, cleavage tears, or vertical tears with secondary lesions that extend into avascular inner
2/3 of meniscus, except in young teen agers;
- ligamentous instability is a relative contraindication to repair;
- see: management of meniscal tears in the ACL deficient knee
- w/ ACL insufficiency, the rate or re-tearing approaches 40%, especially in younger acitve individuals, and therefore
ACL reconstruction should be performed at the same surgery;
- ref: Arthroscopic meniscal repair using an exogenous fibrin clot.
Surgical techniques for arthroscopic meniscal repair.
- horizontal cleavage tear:
- The repair of horizontal cleavage tears yields higher complication rates compared to meniscectomy: a systematic review.
- Meniscal repair associated with a partial meniscectomy for treating complex horizontal cleavage tears in young patients may lead to excellent long-term outcomes.
- Arthroscopic All-Inside Repair of Medial Meniscus Grade 2 Horizontal Cleavage Tear Using Additional Posteromedial Portal.
- Vertical Lasso and Horizontal Lasso Sutures for Repair of Horizontal Cleavage and Horizontal Oblique Meniscal Tears: Surgical Technique and Indications.
- Platelet-Rich Fibrin Clot-Augmented Repair of Horizontal Cleavage Meniscal Tear.
- Circumferential Suture Repair of Isolated Horizontal Meniscal Tears Augmented With Fibrin Clot.
- Horizontal Cleavage Meniscus Tear Treated With All-inside Circumferential Compression Stitches
- Management of traumatic meniscal tear and degenerative meniscal lesions. Save the meniscus
- Changes in Contact Area in Meniscus Horizontal Cleavage Tears Subjected to Repair and Resection
- Repair of isolated horizontal meniscal tears with all-inside suture materials using the overlock method: outcome study with a minimum 2-year follow-up
- Meniscal Repair of Degenerative Horizontal Cleavage Tears Using Fibrin Clots: Clinical/Arthroscopic Outcomes in 10 Cases.
- Arthroscopic repair of horizontal meniscal cleavage tears with marrow-stimulating technique
- Repair of horizontal meniscus tears: a systematic review.
- Clinical outcomes of open meniscal repair of horizontal meniscal tears in young patients
- Repair of horizontal meniscal cleavage tears with exogenous fibrin clots
- A Prospective, Randomized, Double-Blind, Parallel-Group, Placebo-Controlled Study Evaluating Meniscal Healing, Clinical Outcomes, and Safety in Patients Undergoing Meniscal Repair of Unstable, Complete Vertical Meniscal Tears (Bucket Handle) Augmented with Platelet-Rich Plasma.
- Technique:
- equipement: (see Arthrex, Mitek, Linvatec, Smith-Nephew)
- single or double barrel cannula system;
- table spoon or small spade retractor;
- long keith needles w/ either 2-0 or O absorable or non absorbable;
- medial repair technique
- lateral repair technique
- meniscal debridement
- outside to in - arthroscopic technique:
- main advantage is that there is a low risk of neurovascular injury, since needles are passed thru precise thru the capsule;
- main disadvantage is that suture placement thru the meniscus may not be precise;
- inside to out - arthroscopic technique:
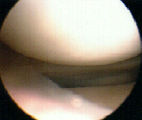
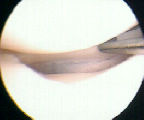
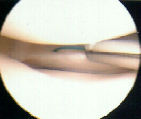
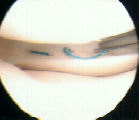

- fibrin clot:
- it was originally recommended that an exogenous blood clot be placed into the meniscal repair site, but this is probably
not necessary;
- Johnson LL (1991) has demonstrated that during and following arthroscopic surgery, blood clot generated during the case
attaches to the surgically incised surfaces (including debrided edges of the meniscal tear);
- w/ this evidence, it may not be necessary to apply and exogenous clot, since the majority of blood clot is formed from
synovial bleeding;
- references:
- Characteristics of the Immediate Postoperative Blood Clot Formation in the Knee Joint.
- Meniscal repair using an exogenous fibrin clot. An experimental study in dogs
- Arthroscopic meniscal repair using an exogenous fibrin clot.
- Preparation of an exogenous fibrin clot.
- suture spacing:
- enough sutures are placed to avoid gaps of more than 3-5 mm;
- sutures can be placed in horizontal, oblique, or verticle direction;
- verticle suture placement may be stronger due to the circumferential orientation of the collagen bundles
(see microscopic anatomy);
- horizontal sutures are almost as strong as verticle sutures, but are more apt to cause eversion of the opposite meniscal surface;
- eversion is avoided by placing sutures on both the superior and inferior mensical surface;
- always place the anterior suture first, so that the view of the posterior suture is not obstructed;
- concomitant ACL reconstruction:
- when performing an meniscal repair along with ACL reconstruction, meniscal repair is done first without tourniquet
followed by ACL reconstruction w/ tourniquet inflated;
- references:
- Failure strengths of different meniscal suturing techniques.
- Meniscus suture techniques: a comparative biomechanical cadaver study.
- The effect of suture type on meniscus repair. A clinical analysis.
- Post Op Rehab:
- Wt bearing as tolerated in brace locked in extension;
- ROM is allowed when not wt bearing;
- atheletics are permited in 4-6 months;
- references:
- Accelerated rehabilitation for meniscus repairs.
- Meniscus repair rehabilitation with concurrent anterior cruciate reconstruction.
- Free rehabilitation is safe after isolated meniscus repair: a prospective randomized trial comparing free with restricted rehabilitation regimens.
Meniscal repair. Description of a surgical technique.
Long-term results of open meniscal repair.
Open meniscus repair. Technique and two to nine year results.
Arthroscopic meniscus repair: a safe approach to the posterior horns.
Failure strengths of different meniscal suturing techniques.
Second look arthroscopy after meniscal repair. Factors affecting the healing rate.
Mitek Omnispan