- Radiographic Evaluation: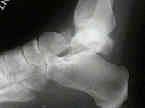
- associated injuries:
- medial malleolus frx (AP view);
- sustentacular tali frx;
- metatarsal head frx;
- its essential to gauge amount of dorsal and medial comminution of talar neck, as well as tendency
for varus angulation;
- Hawkins Classification
- type I talar fractures
- type II talar fractures
- type III talar fractures
- Treatment:
- see: operative treatment
- closed reduciton attempt after x-rays;
- emergent ORIF all open/unreducible fxs;
- attempt reconstruction / avoid arthrodesis;
- use rigid, interfragmentary compression screws (3.5, 4.0, 6.5 mm)
- goal of frx treatment with talar neck fractures is to restore neck to its anatomic position and also to check for varus or supination
malalignment of talar neck;
- because supination forces in Class II and Class III injuries cause subluxation of the subtalar joint, it is important to ensure that
subtalar joint has been reduced completely;
- an increased incidence of fractures of medial malleolus has been reported with type II and III fractures;
- malunion is avoided by open anatomic reduction & internal fixation.
- w/ incomplete reduction, varus hindfoot & dorsal displacement are most common;
- dorsal displacement leads to limited dorsiflexion & may be salvaged by dorsal beak resection.
- symptomatic varus deformity is likely to require triple arthrodesis.
- Results:
- infection - rare in closed injuries;
- avascular necrosis
Hawkins 1: 0- 13%
Hawkins 2: 20- 50%
Hawkins 3: 20-100%
- problem - precision of dx: Hawkins Sign helpful if present at 6-8 weeks;
- arthritis - 40-90%
- related to articular damage, subchondral collapse (from AVN), immobilization, and malunion;
- non union of talar frx:
- frx healing is somewhat less of problem than might be expected w/ this injury;
- delayed union ( > 6 mo after injury) is common, but nonunion is relatively rare;
- delayed unionn - upto 15%; Non Union rare; both decreased with ORIF;
- in the report by Elgafy H, et al (2001), 58 patients with 60 talar fractures were retrospectively reviewed;
- 27 (45%) of the fractures were neck, 22 (36.7%) process, and 11 (18.3%) body;
- 48 fractures had operative treatment and 12 had non-operative management;
- average follow-up period was 30 months (range, 24-65);
- 32 fractures (53.3%) developed subtalar arthritis (but only 2 patients had subsequent subtalar fusion);
- 15 fractures (25%) developed ankle arthritis (none of these patients required ankle fusion);
- fractures of the body of the talus were associated with the highest incidence of DJD of both the subtalar and ankle joints;
- 10 fractures (16.6%) developed avascular necrosis (AVN), only one of which had subsequent slight collapse;
- avascular necrosis occurred mostly after Hawkins Type 3 and 2 fractures of the talar neck;
- assessment with the three rating scores showed that the process fractures had the best results followed by the neck and then
the body fractures;
- varus malunion:
- can be difficult to recognize when treating talar neck fractures;
- may be cause by medial screw compression w/ medial neck comminution;
- varus position limits subtalar motion;
- may cause subtalar arthrosis and pain;
- ref: Outcomes of Talar Neck Fractures: A Systematic Review and Meta-analysis.
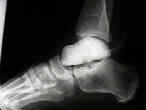 - Salvage:
- Salvage:
- Type IV:
- subtalar, tibiotalar, and talonavicular joint subluxation or dislocation;
- talar neck fracture w/ dislocation of the head fragment;
- open type IV fractures are associated w/ high rate of infection (30%), despite aggressive debridement
and infection;
- salvage treatment:
- consider placement of methylmethacrylate spacer shaped like a talus;
- there are documented cases of patients being pain free for several years with this method of treatment
Fractures of the talus: experience of two level 1 trauma centers.
Treatment of talar neck fractures: clinical results of 50 patients.
Surgical treatment of talus fractures: a retrospective study of 80 cases followed for 1-15 years.
Talar Neck Fractures: Results and Outcomes.
Open Reduction and Stable Fixation of Isolated, Displaced Talar Neck and Body Fractures.
Direction of the oblique medial malleolar osteotomy for exposure of the talus

