- Discussion:
- in the presence of H.O. the nerve should be placed in the subcutaneous position, since H.O. forms between muscle layers;
- sub-muscular transposition (or subQ transposition) is also indicated to relieve tension following ulnar nerve repairs;
- is often indicated in revision cubital tunnel surgery;
- may be the procedure of choice in cases of moderately severe entrapment (from Dellon, et al (1989))
- Review of treatment results for ulnar nerve entrapment at the elbow.
- Anatomy & Sites of Compression
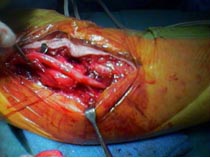
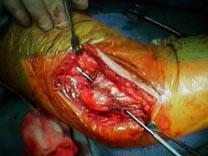
- Technique:
- gentle curving incision placed 1 cm behind epicondyle;
- posterior branches of medial antebrachial cutaneous nerve may be found at the level of the epicondyle;
- ulnar nerve is identified proximally and posteriorly and is followed distally;
- consdier possible points of compression;
- distal segment of medial intermuscular septum is excised, just above the medial epicondyle;
- flexor pronator origin: (forearm flexors)
- ulnar nerve is retracted out of the way;
- flexor-pronator origin is incised off the epicondyle, leaving a cuff of tissue for later repair;
- care is taken not to injure the MCL which originates off the base of the medial epicondyle;
- nerve is transposed beneath the flexor pronator muscle mass (next to the median nerve);
- flexor pronator origin is re-attached to the medial epicondyle;
- ensure that iatrogenic nerve compression is not present;
- some authors recommend that the surgeons gloved little finger should be able to pass between the nerve and repaired tendon;
- alternatives:
- z lengthening of the flexor pronator mass:
- motivation is to avoid tension on the transposed nerve by the flexor pronator mass;
- this technique may be best suited for patients with moderately severe cubital tunnel syndrome;
- in the study by Nouhan and Kleinert (1997), 36% of patients had a an excellent result and 61% had a good result;
- technique involves division of the flexor pronator mass in a step cut fashion w/ care taken to avoid injury to the ulnar collateral nerve;
- ulnar nerve is transposed to lie next to the median nerve;
- the lengthened flexor pronator mass is sutured back to its origin;
- intra-muscular transposition:
- involves transection of the fascia 1 cm from the medial epicondyle and division of 1/2 the muscle mass;
- the nerve is placed in a circumferential bed of muslce;
- outcomes:
- in the series by Leone J, et al (2001), a consecutive series of 39 anterior intramuscular transpositions were reviewed;
- results showed early clinical improvement of 77% of patients (mean follow-up, 3.34 months);
- with repeated assessments later, the same group of patients had clinical improvement of 62% (mean followup, 30.9 months);
- patients younger than 50 years, individuals who underwent external neurolysis, or patients who had a previously failed
subcutaneous transposition had fewer satisfactory results
- Ulnar nerve decompression by transposing the nerve and Z-lengthening the flexor-pronator mass: clinical outcome.
- Anterior intramuscular transposition with ulnar nerve decompression at the elbow.
Submuscular Transposition of the ulnar nerve.
The failed ulnar nerve transposition. Etiology and treatment.
Technical problems with ulnar nerve transposition at the elbow: Findings and results of reoperation.
Anterior submuscular transposition of the ulnar nerves by the Learmonth technique.
Submuscular Transposition of the Ulnar Nerve.
Review of treatment results for ulnar nerve entrapment at the elbow.
Anterior Intramuscular Transposition With Ulnar Nerve Decompression at the Elbow.
Anterior intramuscular transposition of the ulnar nerve for cubital tunnel syndrome.