- Mosaicplasty:
- refers to the technique of harvesting small circular (4-8 mm) autogenous grafts from the knee from non wt bearing regions of the knee, and transplanting the grafts in a mosaic pattern until the osteochondral defect is filled;
- typically the grafts are harvested from the periphery of the supero-lateral trochlea, but often, the superomedial portion of the trochlea will be used if upto 15 grafts are required;
- indications:
- classic indication include patients less than 45 years, with moderate sized chondral or osteochondral defects but less than 2 cm;
- outcome studies:
- A prospective randomized clinical study of mosaic osteochondral autologous transplantation versus microfracture for the treatment of osteochondral defects in the knee joint in young athletes
- histology:
- in the report by Barber FA, et al, the authors report on the histology of clinical cases obtained at intervals from 2 to 12 months after arthroscopic osteochondral transplantation;
- patients found at arthroscopy to have full-thickness femoral condyle defects between 1 and 3.5 cm in diameter underwent arthroscopic osteochondral transplantation;
- at various time intervals from 2 to 12 months after the osteochondral transplantation, arthroscopic biopsy specimens of the recipient sites were obtained;
- 7 patients underwent biopsy at intervals ranging up to 12 months postoperatively;
- all showed maintenance of the integrity of the grafts with living chondrocytes and osteocytes;
- donor sites filled without grafting and were covered with fibrocartilagenous scar;
- references:
- Arthroscopic osteochondral transplantation. Histologic results.
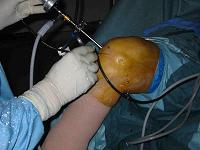
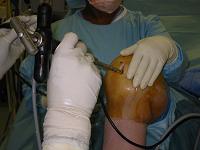
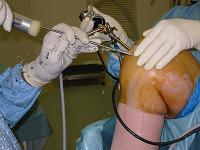
- Surgical Technique:
- peripatellar incision:
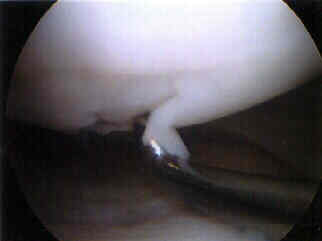
- the surgeon inserts a spinal needle thru the mid aspect of the patellar incision and the surgeon then directs the needle toward the lateral aspect of the intercondylar notch and toward the medial femoral chondral lesion;
- the peripatellar incision which allows the best perpendicular approach to both surfaces is selected;
- the surrounding fat pad is taken down with a motorized shaver;
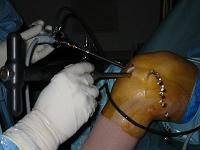
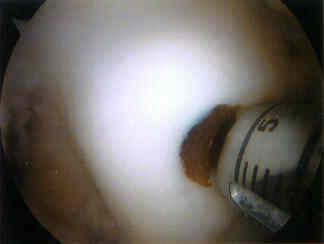
- donor site harvest:
- grafts are usually 4-8 mm in diameter and 15-20 mm deep;
- grafts taken from the superior and lateral intercondylar femoral notch;
- the knee is flexed or extended to place the harvesting tube perpendicular to the articular surface;
- hyperflexion of the knee allows harvest at the far inferior aspect of the lateral intercondylar notch;
- as an alternative, the superomedial portion of the trochlea will be used if additional are required;
- harvest tunnels are kept 1-2 mm apart;
- fibrocartilage will fill in the residual defects;
- reference:
- Primary stability of osteochondral grafts used in mosaicplasty.
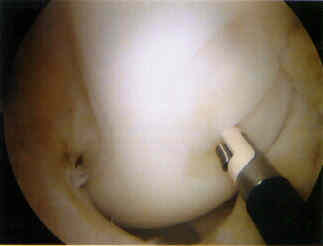
- recipient site:
- use either the peripatellar incision or the medial portal site, depeding on which allows the most perpendicular direction;
- use knee flexion/extension to achieve the best perpendicular direction;
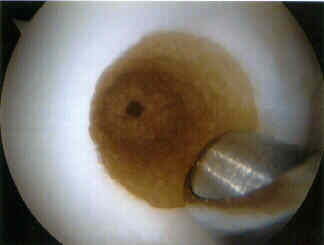
- impaction type drill is used to drill out defect;
- drill depth is taken 5 mm deeper than the harvest graft length;
- cancellous bone bridges were maintained between drill holes;
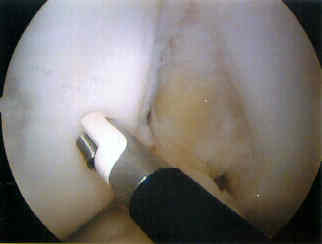
- graft delivery:
- care is taken to deliver the graft in the exact direction as the drill hole;
- once the graft has bee delivered, a tamp is often needed to gently nudge the graft flush with the surrounding cartilage;
- references:
- Effects of Small Incongruities in a Sheep Model of Osteochondral Autografting.
- Effect of Impact on Chondrocyte Viability During Insertion of Human Osteochondral Grafts.
- The Effect of Angled Osteochondral Grafting on Contact Pressure. A Biomechanical Study.
- post op care:
- patients are kept non wt bearing for 4-6 weeks postop;
- custom fitted valgus unloading knee braces are used whenever possible;
- aggressive patellar mobilization is required inorder to prevent patellar arthrofibrosis;
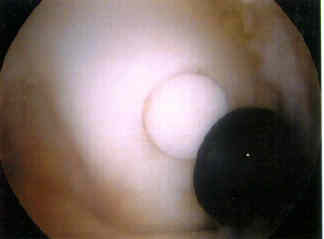
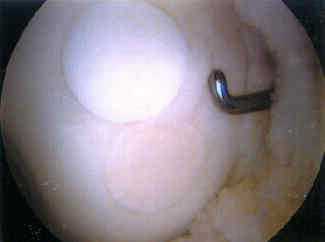
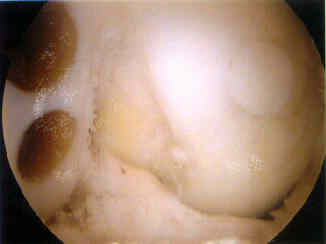
- case example
- 38-year-old male who underwent osteochondral grafting for a full thickness chondral injury;
- 1 1/2 years after surgery, he had recurrent pain over the medial femoral condyle and a second look arthroscopy demonstrated that the original graft was intact, however, there was an extension of the chondral injury inferior to the graft which required additional grafting;
- Cartilage Transplants: (see carticel)
- in young adults w/ large chondral lesions involving the wt bearing portions of the knee, consider reduction and fixation of the displaced fragment if possible or alternatively consider the controversial technique of preserved chondral allografting;
- in the report by Breinan, et al. (1997), no differences in healing could be detected between dogs which had injection of cultured autologous chondrocytes (under a periosteal flap) versus a control group;
- references:
- Effect of cultured autologous chondrocytes of repair of chondral defects in a canine model.
- Durability of regenerated articular cartilage produced by autogenous periosteal grafts in major full-thickness defects in joint surfaces under influence of continuous passive motion. A follow-up report at one year.
- Treatment of deep cartilage defects in the knee with autologous chondrocyte transplantation.
- A Randomized Trial Comparing Autologous Chondrocyte Implantation with Microfracture. Findings at Five Years
Isolated chondral fractures of the knee.Bauer JJ. Arthoscopic Rel Surg. 1988
Mesenchymal Cell Based Repair of Large Full Thickness Defects in Articular Cartilage.
Restoration of injured or degenerated articular cartilage.
Osseous injury associated with acute tears of the anterior cruciate ligaments.
Spontaneous repair of superficial defects in articular cartilage in a fetal lamb model.
Autologous Osteochondral Grafting in the Knee: Indication, Results, and Reflections.
Mosaicplasty for the treatment of articular cartilage defects: application in clinical practice.
Mosaicplasty for the Treatment of Articular Defects of the Knee and Ankle.
Biomechanical and Histological Evaluation of Osteochondral Transplantation in a Rabbit Model.
The Effect of Graft Height Mismatch on Contact Pressure Following Osteochondral Grafting.
The effect of graft sizing on osteochondral transplantation.
Mechanical Behavior of Articular Cartilage After Osteochondral Autograft Transfer in an Ovine Model.
Contact Pressure Comparison of Proud Osteochondral Autograft Plugs Versus Proud Synthetic Plugs