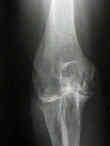
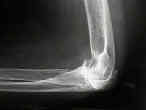
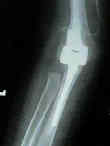
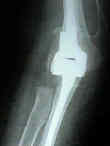
- Discussion:
- up to 80 % of patients w/ traumatic DJD may expect a good to excellent result at 5 years;
- up to 30 % of patients will sustain a major complication over 5 years, which often will require and additional operation;
- indications:
- end stage rheumatoid arthritis;
- severe intractable pain in association with severe grade 3,4,5
- major cysts at olecranon-coronoid junction, in association w/ severe grade 3-5 erosions;
- progressive loss of extension beyond 60 deg;
- instability which indicates very severe bone destruction and endangered ligamentous stability;
- fracture:
- comminuted humeral intercondylar fracture in patients over age 70;
- long term results may be unpredictable:
- references:
- Distal humeral fractures treated with noncustom total elbow replacement.
- Distal humeral fractures treated with noncustom total elbow replacement. Surgical technique.
- A comparison of open reduction and internal fixation and primary total elbow arthroplasty in the treatment of intraarticular distal humerus fractures in women older than age 65.
- Primary total elbow replacement for fractures of the distal humerus.
- Total elbow arthroplasty for non-rheumatoid patients with a fracture of the distal humerus: a minimum ten-year follow-up.
- Preoperative considerations:
- if there is also significant RA involvement of the shoulder the question is which joint should be adressed first;
- many authors will prefer to perform the total elbow arthroplasty before the TSR;
- allows greater amount of time between arthroplasties and allows greater functional improvement;
- in addition w/ concomitant disease in both joints, it can be difficult to judge humeral retroversion (due to loss of
ligamentous contrainsts in elbow;
- need for semiconstrained prosthesis:
- patients who have had previous radial head resection and synovectomy (if unconstrained prosthesis is used);
- severe ligamentous laxity (if unconstrained prosthesis is used);
- more than 2 cm of distal humeral bone loss (may require customized prosthesis)
- references:
- Total elbow arthroplasty after previous resection of the radial head and synovectomy.
- Results of TEA after excision of the radial head and synovectomy in patients who had rheumatoid arthritis.
- Technique: (using the Coonrad-Morrey prosthesis - semiconstrained); (Discovery™ Elbow System)
- posterior triceps reflecting approach:
- tendon splitting approach: tendon insertion to the proximal ulna is elevated from the medial and lateral aspects of the ulna,
keeping the forearm fascia extending to the proximal ulna intact;
- alternatively, medial half of triceps is reflected along w/ posterior capsule, and the extensor mechanism is reflected laterally;
- ulnar nerve is identified and is transposed anteriorly;
- ligamentous release:
- both collateral ligaments may be released off of epicondyles if a semiconstrained prosthesis is used (such
as semiconstrained modified Coonrad-Morrey);
- anterior capsule release:
- anterior capsule is released from the distal humerus to fully expose the joint and release any contracture;
- tip of the olecranon (and coronoid tip) is removed along w/ a portion of the MCL to gain better exposure;
- exposure is adequate when the lateral column is exposed;
- reference:
- The osteo-anconeus flap. An approach for total elbow arthroplasty.
- The Lateral Para-Olecranon Approach for Total Elbow Arthroplasty
- humeral preparation:
- if humerus is prepared first then realize, then ulna is often smaller and may dictate sizing options;
- only the diaphysis is needed for secure fixation of the humeral component;
- deficiency or absence of an epicondyle should not be major problem;
- medullary canal is entered w/ a twist reamer and is exchanged for alignment stem w/ attached cutting block (placed radially);
- cutting block: set to remove an appropriate amount of distal humerus;
- consider seating the humeral component more proximal than usual to help relax the anterior soft-tissue envelope in extension
- ref: Effect of humeral condylar resection on strength and functional outcome after semiconstrained total elbow arthroplasty.
- controversies:
- cement vs press fit stems:
- in the report by Kudo H, et al (1999), the authors advocate press fit fixation with a circumferential plasma spray
fixation of the humeral component;
- humeral fixation with a concomitant shoulder arthroplasty:
- in report by Gill et al., the authors recommended filling IM canal with cement if the interval between the humeral
component stems is less than 6 cm);
- ref:
- Primary Souter-Strathclyde Total Elbow Prosthesis in Rheumatoid Arthritis.
- Ipsilateral total shoulder and elbow arthroplasties in patients who have rheumatoid arthritis.
- ulnar preparation:
- olecranon tip is removed to gain straight-line access to the canal;
- medullary canal is entered w/ a high speed drill;
- the previously removed olecranon tip facilitates entry into the canal;
- sequential rasping is performed w/ care to avoid proximal ulnar complication;
- broach parallel to the dorsal cortex to avoid malalignment;
- in the report by Kudo H, et al (1999), the authors advocate use of an all polyethylene cemented ulnar component;
- Primary Souter-Strathclyde Total Elbow Prosthesis in Rheumatoid Arthritis.
- cement insertion:
- consider adding one gram of tobramycin to the cement (see addition of antibiotics to cement)
- use a cement gun to insert cement;
- cement is allowed to harden w/ the elbow in extension;
- component insertion:
- ulnar component is articulated w/ the humeral component before the humeral component is seated;
- bone graft is placed behind the anterior humeral component falange;
- this helps the humerus resist posterior displacement and rotational displacement;
- remember that maximal stresses are found anteriorly at the insertion site of the humeral component, and that after bone
graft incorporates, thickened cortex will help resist these forces;
- humeral component is impacted down the medullary canal;
- ulnar component is inserted;
- wound closure:
- triceps should be reattached w/ intra-osseous sutures, which are inserted prior to component insertion;
- repair of the collateral ligaments is not necessary;
- consider maintaining the elbow in extension for 2-3 days in order to allow the soft tissues to heal;
- Complications:
- posterior elbow dislocation;
- may occur in approximately 10% of patients undergoing unconstrained arthroplasty;
- ulnar nerve dislocation;
- impingement of the radial head;
- proximal ulna fracture;
- hardware failure:
- worn bushings;
- fracture of ulnar component;
- infection:
- may range from 1 to 10%;
- in acute infection w/ non virulent organism (not staph epidermidis) approximately 50% of patients may expect successful
outcome from multiple debridements and retention of components;
- as a requirement for this technique all bushing need to be removed in order to allow a thorough washout;
- staged removal of components, debridements, and re-implantation of components will be successful in the majority of patients
if highly virulent organisms are not present (such as stap epidermidis);
- staph epidermidis infections are expected to recur if components are re-inserted;
- resection arthroplasty should result in the erradication of infection and will provided relatively high rates of patient
satisfaction (despite poor function);
- references:
- Management of infection about total elbow prostheses.
- Infection after total elbow arthroplasty.
Current Concepts Review: Total Elbow Arthroplasty.
Total elbow arthroplasty for complete ankylosis of the elbow.
Capitellocondylar total elbow replacement. A long-term follow-up study.
Salvage of non-union of supracondylar fracture of the humerus by total elbow arthroplasty.
Primary semiconstrained total elbow arthroplasty. Survival analysis of 113 consecutive cases.
Total elbow arthroplasty. An 18-year experience.
Primary degenerative arthritis of the elbow. Treatment by ulnohumeral arthroplasty.
Strength function after elbow arthroplasty.
Capitellocondylar total elbow arthroplasty. Two-to eight-year experience.
Semiconstrained elbow prostheses with special reference to the GSB III prosthesis.
Capitellocondylar total elbow replacement. A long-term follow-up study.
Semiconstrained arthroplasty for the treatment of rheumatoid arthritis of the elbow.
Capitellocondylar total elbow replacement in rheumatoid arthritis.
Capitellocondylar total elbow replacement in rheumatoid arthritis. Long-term results.
Semiconstrained arthroplasty for the treatment of rheumatoid arthritis of the elbow.
Motion and laxity of the capitellocondylar total elbow prosthesis.
Total elbow arthroplasty in patients who have juvenile rheumatoid arthritis.
Débridement Arthroplasty for Primary Osteoarthritis of the Elbow
Primary Souter-Strathclyde Total Elbow Prosthesis in Rheumatoid Arthritis.
Results of reconstruction for failed total elbow arthroplasty.