- Operative Considerations (see IM nailing and Synthes IM Nail);
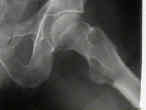
- should be considered when x-rays show more than 50% loss of the shaft diameter on any view;
- risk of pathologic frx is low for lesions involving 50% of the shaft diameter (assuming that patient is touch down weight bearing), but rises dramatically
after the lesion involves more than 75% of the shaft diameter;
- pitfalls:
- prior to IM nailing for pending pathologic frx, it is necessary to ensure that the lesion in question is in fact a carcinoma rather than a sarcoma (such
as chondrosaroma) which have disasterous consequences if a nail were driven thru it;
- one should be especially suspicious with the mixed lytic/blastic type lesion (as may be seen in breast or prostatic ca);
- term "millary sarcomatous metatasis" has been given to cases in which an IM nail has been driven thru a femoral sarcoma (the lung
is filled with countless sarcomatous metatasis);
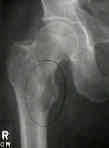
- lesser troch avulsion is not an uncommon presentation of metastatic bone dz, but has also been described as initial indicator of chondrosarcoma;
- reference: Avulsion Fracture of the Lesser Trochanter as a Result of a Primary Malignant Tumor of Bone. A report of four cases.
- bone scans
- help pick up additional metastatic lesions, and may lesions which were not noticed on plain radiographs;
- if operative fixation of a pending femoral shaft frx is planned, we need to know whether there is metatstatic involvement in proximal or distal femur;
- prophylaxis against FES:
- note that patients w/ lung carcinoma or w/ significant metatasis to the lungs may be especially sensitive to fat embolism syndrome;
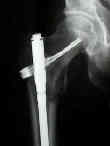
- intramedullary nails are inserted without femoral reaming;
- bilateral IM nailing should be done with caution (FES rates may reach 100%);
- preoperative steroids:
- hydrocortisone 100 mg IV q6 hrs which is started the evening before the case;
- references:
- Fat embolism prophylaxis with corticosteroids. A prospective study in high-risk patients.
- 'Low-dose' corticosteroid prophylaxis against fat embolism.
- Fat embolism and the fat embolism syndrome. A double-blind therapeutic study.
- The use of methylprednisolone and hypertonic glucose in the prophylaxis of fat embolism syndrome.
- canal venting:
- the femur is most efficiently vented by inserting a cannulated femoral nail without a guide wire;
- proof of femoral venting is revealed when the medullary contents are extruded from proximal end of nail, as the nail is driven forward;
- prior to insertion of the IM nail, consider venting the medullary canal inorder to avoid FES;
- make a stab wound over the distal metaphyseal-diaphyseal junction and spread down to bone;
- insert a 4.0 mm cannulated drill bit over a guide wire into the medullary canal;
- references:
- Intramedullary pressure changes and fat intravasation during intramedullary nailing: an experimental study in sheep.
- Novel Venting Technique for Intramedullary Rod Fixation of Pathologic Fractures
- radiation therapy
- outcomes:
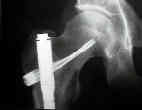
- in the report by M. Assal et al 2001, the authors evaluated 12 pathologic and impending pathologic fractures which were
stabilized with the synthes spiral blade plate;
- two patients required bilateral nailing which was staged over 2-3 weeks;
- average post surgical survival was 6 months;
- one patient died during surgery from a fat embolism;
- the authors noted that although nails were inserted without reaming, this did not avoid the risk of fat embolism
Metastatic bone disease. A study of the surgical treatment of 166 pathologic humeral and femoral fractures.
Isolated fracture of the lesser trochanter in adults: an initial manifestation of metastatic malignant disease.
Metastasis size in pathologic femoral fractures.
Osteosynthesis of metastatic lesions of the proximal femur with a solid femoral nail and interlocking spiral blade inserted without reaming.
Cardiopulmonary complications of intramedullary fixation of long bone metastases.
Intramedullary Nailing of (Impending) Pathologic Fractures.
Intramedullary nails for long bone metastases: why do they fail?