- See:
- Phalangeal Injury
- Congenital Trigger Thumb
- Rheumatoid Trigger Finger 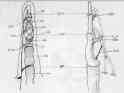
- Discussion:
- results from localized tenosynovitis of superficial and deep flexor tendons adjacent to A1 pulley
at a metacarpal head;
- inflammation causes nodular enlargement of tedon distal to pulley;
- occurs most often in middle or ring fingers (occassionally in thumb);
- rheumatoic trigger finger may involve several fingers;
- prognostic factors:
- diabetes is a poor prognostic indicator for nonoperative treatment;
- these patients may also be especially prone to develop stiffness following surgical release;
- probably the most important prognositic indicator of good results w/ non operative treatment is the duration of triggering
prior to treatment;
- irreducibly locked trigger, often w/ flexion contracture of PIP joint, should certainly not be treated by injections;
- associated disorders:
- RA, gout, diabetes, amyloidosis;
- diff dx:
- triggering at decussation of superficial flexor over the deep flexor;
- MP joint locking
- FDP avulsion/rupture:
- failure of digit extension from chronic dislocation of mcp
- pt can maintain extension achieved passively
- bouvier's test
- post interosseous nerve syndrome: tenodesis effect present - not present with rupture
- trigger finger (no passive movement possible);
- extensor tendon rupture
- saggital band rupture:
- with saggital band rupture the patient will maintain full passive motion of the MP, PIP, and DIP joints;
- thumb sesamoid bone:
- ref: Painful Clicking of the Thumb Interphalangeal Joint Caused by a Sesamoid Bone: A Report of Three Cases
- Clinical Manifestations:
- occurs most often in long or ring fingers (occassionally in thumb)
- produces a painful clicking as inflammed tendon passes thru constricted sheath as finger is flexed and extended;
- digit may lock in flexion, extension, or may be arrested in the middle range;
- determine if there is normal passive ROM in the MP, PIP, and DIP joints (with true triggering there should be locking as the digit is
passively taken thru a ROM);
- w/ chronic triggering, a PIP flexion contracture (or IP flexion joint contracture) may develop;
- palpation may reveal tender nodule over metacarpal head (which may imply a better prognosis w/ nonoperative treatment);
- determine if the patient can flex and extend the digit past the triggering point w/o assistance;
- Non Operative Treatment:
- dutifully applied non operative treatment should cure well over 95% of trigger finger patients in a general orthopaedic practice;
- Percutaneous Technique:
- in report by Gilberts et al, authors compared results of an open surgical technique with those of a percutaneous technique for
treatment of trigger digits;
- 96 patients/100 trigger digits randomized to either open (n = 46) or percutaneous (n = 54) surgical release of 1st annular pulley;
- digits were successfully treated in 98% of open surgical technique and in 100% of the cases using the percutaneous technique;
- mean operation time was significantely longer using the open technique;
- mean duration of postoperative pain and time to recovery of motor function were significantely shorter for patients treated with
the percutaneous method;
- no serious complications were observed in either group;
- references:
- Percutaneous release of trigger digit with and without cortisone injection.
- Percutaneous release of the trigger finger: an office procedure.
- Closed division of the flexor tendon sheath for trigger finger.
- Prospective randomized trial of open versus percutaneous surgery for trigger digits
- Operative Considerations:
- rheumatoid trigger finger:
- incising A1 pulley may cause bowstringing of tendon & deviation of finger toward midline & propencity for
anterior MCP subluxation;
- resect one slip of FDS (if necessary for gluiding)
- Surgical Approach:
- local anesthesia:
- allows patient to actively flex & extend digit to verify complete release;
- see: median nerve block and ulnar nerve block;
- anatomy:
- average length of A1 pulley is 1 cm;
- proximal edge of the 1st annular pulley lies about 2 cm from the proximal finger crease;
- distal edge of A1 pulley lies about 1 cm from the proximal finger crease;
- note that the proximal phalangeal crease which lies over the mid portion of the proximal phalanx, and that the A2 pulley begins
and ends in the proximal half of the proximal phalanx;
- hence, a tendon sheath incision which extends past the level of the proximal phalangeal crease
will probably incise most the A2 pulley; 
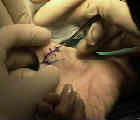
- incision:
- transverse 15 mm incision is made over the affected metacarpal neck, or can be made w/
reference to the palmar creases mentioned above;
- once skin has been incised, use blunt dissection to spread subQ tissue and palmar fascia
to expose flexor tendons and sheath;
- incision must not violate distal palmar flexion crease
- spread thru the plamar fascia w/ a dissecting tonsil, and apply to small blunt retrators, which
should expose the tendon;
- ref: Comparison of 3 different incision techniques in A1 pulley release on scar formation and postoperative rehabilitation
- identify the digital nerves:
- nerves lie on either side of the tendon sheath;
- usually radial nerve is more vulnerable;
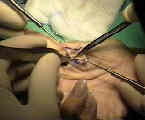
- transection of pulley:
- its essential to identify the demarcation between the A1 and A2 pulleys;
- insert an anatomy probe into this interval, and then pass it proximally underneath the A1 pulley;
- A1 pulley should be split longitudinally along radial aspect of pulley (in index, long, & ring fingers) and along ulnar aspect of
little finger);
- this help prevent subluxation of flexor tendons;
- release only enough pulley, to allow full active motion w/o triggering;
- at the end of the procedure, move the finger to ensure that there is no more triggering;
- look for tendon pathology:
- consider delivering the tendon out of its sheath using a small right angle rectractor;
- if a nodule is present, a piece of the tendon sheath may need to be excised to allow passage of the tendon;
- Trigger Thumb:
- thumb tendon sheath anatomy:
- A1 pulley: spans the MP joint, approximately 8 mm in width;
- note that the FPB inserts just proximal to this pulley and the adductor pollicis inserts distal to the A1 pulley;
- oblique pulley: located over the mid aspect of the phalanx, approximately 10 mm in width;
- note that the adductor pollicis partially inserts into the oblique pulley;
- A2 pulley located at the most distal aspect of the proximal phalanx, and is 9 mm in width;
- it may partially span the thumb IP joint;
- incision:
- proximal edge of the FPL longus sheath annulus is directly deep to the MP flexion crease of the thumb;
- hence, a transverse incision should be made at the MP flexion crease or just distal to it;
- note position of lateral (radial) digital nerve to thumb in position of jepardy;
- radial nerve lies close to deep layer of dermis at flexion crease;
- radial nerve can be injured by blunt dissection more proximally where it diagonally crosses thumb flexor sheath;
- Post Op:
- recognized that adhesions may form if the patient does not begin immediate motion
Trigger fingers and thumb: when to splint, inject, or operate.
Pathobiology of the human A1 pulley in trigger finger.
Results of surgery for trigger finger.
Bowstringing as a complication of trigger finger release.
Injection versus surgery in the treatment of trigger finger.
The results of surgical treatment of trigger finger.
Trigger Digits: Principles, Management, and Complications.
Surgical Treatment of the Pediatric Trigger Finger
A Historical Perspective of the Notta's Node in Trigger Fingers