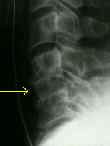
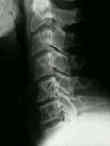
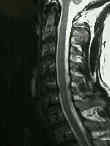
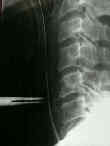
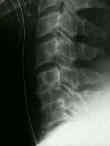
- See: Anterior Approach to Cervical Spine:
- Discussion:
- Smith Robinson disectomy & block fusion is preferred over Cloward dowel for involvement of one or two interspaces;
- for multi-level spondylosis & myelopathy, w/ more extensive anterior decompression involving excision of osteophytes & multiple
vertebrectomies, a strut graft fusion is indicated;
- PreOperative Considerations:
- attention to sagittal alignment is important;
- maintain physiological lordosis at segment or segments involved in arthrodesis;
- kyphosis:
- long-standing localized angular kyphosis resulting from inadequate bone-grafting or graft subsidence may lead to recurrence of
myelopathy from stenosis at adjacent levels;
- Anterior Approach:
- see: anesthetic considerations
- anatomy:
- carotid tubercle:
- carotid tubercle is located on the anterolateral aspect of c6;
- longus capitis and anterior scalene muscles attach to it;
- vascular structures:
- inferior thyroid artery course horizontally toward midline as branch as branch of thyrocervical trunk at the level of C7;
- vertebral arter is posterior, the omohyoid origin is superior;
- left lymphatic duct is posteroinferior;
- internal jugular vein is lateral;
- Bone Graft Techniques:
- see bone grafts harvest technique;
- Cloward:
- dowel graft technique;
- Robsinson technique:
- rectangular iliac crest;
- grafts of 6-7 mm in height are ideal;
- larger grafts may cause excessive distraction and are at risk for anterior extrusion;
- Distraction: (for spondylosis)
- anterior interbody arthrodesis allows distraction of collapsed disc, which opens foramina & decompressing nerve roots;
- distraction places tension on ligamentum flavum, which reduces invagination of this structure into canal;
- excessive distraction is not attempted because it can result in harmful tension on the spinal cord;
- it is difficult to decompress nerve root directly in foramen thru anterior approach;
- Internal Fixation:
- advantages of internal fixation include maintenance of spinal alignment, improvement of stability of graft construct, & elimination for
need of halo in selected patients;
- note that even in experienced hands, hardware failure is not uncommon;
- includes loosening of the screw or plate or screw breakage;
- other complications include, screw pentration of disc space, and insertion of excessively long screws;
- Post Op:
- after corpectomy, use halo to maintain proper position;
- catastrophic neurological injury can result from strut graft dislodgment;
- Complications:
- neurologic injury (<1 %);
- injury to the recurrent laryngeal nerve may occur if the right sided approach is used;
- anterior graft migration:
- more common after multi-level fusions;
- more common w/ excessive disc heights (more than 9 mm) and excessive distraction;
- pseudoarthrosis:
- may result from graft collapse w/ resultant kyphosis and neurologic change;
- by definition pseudoarthrosis is present when there is radiolucency at the fusion level or more than 2 mm of motion at the fusion site;
- frequency:
- ranges from 4 to 20% for single level fusion;
- ranges from 27 to 50% for multilevel fusion;
- management:
- if patient is asymptomatic and no deformity is present, then consider prolonged trial of semi-rigid collar;
- if patient is symptomatic, consider posterior fusion and spinous process wiring or with repeat anterior arthrodesis;
- references:
- Treatment of symptomatic anterior cervical nonunion using the Rogers interspinous wiring technique.
Complications of fusion to the upper cervical spine.
Fusion of the upper cervical spine in children and adolescents. An analysis of 17 patients.
Nonunion following two-level anterior cervical discectomy and fusion.
Complications of anterior cervical disk removal and fusion.
Fracture-dislocations of the cervical spine. Instability and recurrent deformity
Anterior cervical plate fixation with the titanium hollow screw plate system. A preliminary report.
Treatment of cervical spine injuries with anterior plating. Indications, techniques, and results.
Failed Anterior Cervical Disectomy and Arthrodesis Analysis and Treatment of 35 Patients.