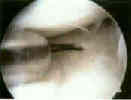
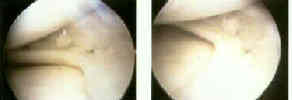
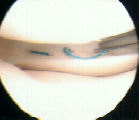
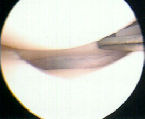
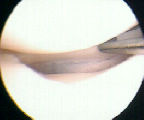
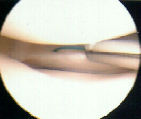
- See: medial meniscus
- Discussion:
- indications:
- any peripheral nondegenerative longitudinal tears < 3 cm;
- if tear is w/in 3 mm of the periphery, it is considered vascular;
- area 3-5 mm from periphery is grey zone, & > 5 mm from periphery is considered avascular; (see vascularity of the meniscus)
- unstable tears or tears within vascular zone that are > 7 mm are repairable;
- mobile, single, vertical, longitudinal tear of the meniscus limited to vascular outer one-third of the meniscal substance;
- note that instability in full extension suggests concomitant POL tear, which by itself is an indication for operative repair (w/ the same incision being used to repair the meniscus);
- relative contra-indications:
- tears greater than 3 cm do not seem to heal, following surgery;
- transverse tears, even in the periphery, do not seem to heal;
- do not repair flap tears, radial tears, cleavage tears, or vertical tears with secondary lesions that extend into avascular inner 2/3 of meniscus, except in young teen agers;
- ligamentous instability is a relative contraindication to repair;
- w/ ACL insufficiency, rate or re-tearing approaches 40%, especially in younger acitve individuals, and therefore ACLR is performed at same surgery;
- ref: Arthroscopic meniscal repair using an exogenous fibrin clot.
Surgical techniques for arthroscopic meniscal repair.
- Technique: (arthroscopy of the knee)
- patient positioning:
- it is essential that the surgeon position the patient so that there is no difficulty in applying a valgus force to the knee while it remains in full extension (ie it does not move into flexion);
- w/o proper positioning, knee will buckle into flexion as a valgus force is applied, and visualization of posterior horn of medial meniscus will be difficult;
- patient is placed in leg holder;
- table is broken just proximal to the knee, and knee is allowed hang free so it can flex to 90 deg;
- it is important to keep the opposite leg abducted (help in a GYN leg holder), so that the surgeon has good access to the medial aspect of the knee (assuming that a medial mensisectomy is being performed);
- some surgeons prefer to perform the meniscal repair in 90 deg of flexion (retracting the saphenous nerve posteriorly, where as other surgeons prefer only slight flexion (retracting the nerve anteriorly);
- exam: note any concomitant medial instability (MCL or POL tears);
- arthroscopic portals:
- it is essential that the arthroscopic portals not be placed too high, otherwise access to the posterior horn of the meniscus will be comprimised;
- w/ posterior horn meniscal tear the scope will remain in the lateral portal and the meniscal repair cannula will be inserted into the medial portal;
- w/ a medial tear of the medial meniscus, the arthoscope should be inserted into the medial portal and the meniscal repair cannula should be inserted into the lateral portal site (this will position the cannula perpendicular to the meniscus);
- incision: (see medial compartment of knee);
- knee is temporarily extended, so a 5 cm verticle incision can be marked over the posteriormedial aspect of the knee (just behind the postero-oblique ligament);
- 5 cm verticle incision over posteromedial corner, with a larger portion of the incision placed below the joint line (often the incision is placed too anterior);
- superficial dissection:
- it is essential to avoid the saphenous nerve which lies posterior to sartorius, and can be located just posterior and distal to the central portion of medial femoral condyle;
- nerve moves anteriorly w/ knee extension and posteriorly w/ knee flexion, and hence knee flexion will help protect the nerve during meniscal repair;
- incise superficial fascia (layer I) along the anterior edge of pes anserinus;
- deep dissection:
- leg is brought into slight flexion;
- pes anserinus and saphenous nerve are retracted posteriorly;
- if necessary, the pes insertion can be partially elevated to provide additional exposure;
- define the interval between the posteromedial capsule and the gastrocnemius;
- the gastroc, and pes tendons (sartorius, semitendinosus, gracilis) are retracted posteriorly and are protected w/ a blunt retractor;
- it is not necessary to dissect the semimembranosus off the capsule and if required, sutures can be placed through the semimembranosus;
- note any possible disruption of the MCL or POL, in which case the torn ends should be tagged for repair at the end of the case;
- outside to in - arthroscopic technique:
- main advantage is that there is a low risk of neurovascular injury, since needles are passed thru precise thru the capsule;
- main disadvantage is that suture placement thru the meniscus may not be precise;
- inside to out - arthroscopic technique:
- advantages: this technique allows for precise placement of sutures in the mensicus;
- disadvantages: this technique does not allow for precise placement of sutures thru the capsule, and therefore there is some potential for neurovascular injury;
- equipement:
- single or double barrel cannula system;
- table spoon or small spade retractor;
- long keith needles w/ either 2-0 or O absorable or non absorbable;
- meniscal debridement:
- fibrin clot:
- it was originally recommended that an exogenous blood clot be placed into the meniscal repair site, but this is probably not necessary;
- Johnson LL (1991) has demonstrated that during and following arthroscopic surgery, blood clot generated during the case attaches to the surgically incised surfaces (including debrided edges of the meniscal tear);
- w/ this evidence, it may not be necessary to apply and exogenous clot, since the majority of blood clot is formed from synovial bleeding;
- reference:
Characteristics of the Immediate Postoperative Blood Clot Formation in the Knee Joint.
- suture passage:
- consider using the anterolateral portal to pass sutures thru the medial meniscus so that the needle will be directed more medially (and hence the risk to posterior neurovascular structures will be minimized);
- sutures may pass through the MCL w/o complication;
- some surgeons prefer to perform the meniscal repair in 90 deg of flexion (retracting the saphenous nerve posteriorly, where as other surgeons prefer only slight flexion (retracting the nerve anteriorly);
- the main disadvantage of flexing the knee to 90 deg is that the sutures may "reef in" the capsular pouch that is present (when the knee is flexed);
- after sutures are placed, flex and extend the knee to ensure that the posteromedial corner has not been reefed (generally reefing the pouch will limit extension);
- sutures are usually tied with the knee in extension;
- suture spacing:
- enough sutures are placed to avoid gaps of more than 3-5 mm;
- sutures can be placed in horizontal, oblique, or verticle direction;
- verticle suture placement may be stronger due to the circumferential orientation of the collagen bundles (see microscopic anatomy);
- horizontal sutures are almost as strong as verticle sutures, but are more apt to cause eversion of the opposite meniscal surface;
- eversion is avoided by placing sutures on both the superior and inferior mensical surface;
- always place the anterior suture first, so that the view of the posterior suture is not obstructed;
- concomitant ACL reconstruction:
- when performing an meniscal repair along with ACL reconstruction, meniscal repair is done first without tourniquet followed by ACL reconstruction w/ tourniquet inflated;
- hazards: when tying down the sutures, be sure that branches of the saphenous nerve are not caught in the suture repair site;
- ref: Arthroscopic meniscal repair using an exogenous fibrin clot.
Surgical techniques for arthroscopic meniscal repair.
- ligament repair:
- at this point in the case, tears of the MCL and/or POL may be repaired;
- Post Op:
- patients require protected weight bearing in brace;
- Wt bearing as tolerated in brace locked in extension;
- ROM is allowed when not wt bearing;
- atheletics are permited in 4-6 months
Meniscal repair. Description of a surgical technique.
Long-term results of open meniscal repair.
Preparation of an exogenous fibrin clot.
Open meniscus repair. Technique and two to nine year results.
The arthroscopic meniscal repair. Techniques and clinical experience.
Arthroscopic meniscus repair: a safe approach to the posterior horns.
Arthroscopic meniscal repair using an exogenous fibrin clot.
Meniscal repair using an exogenous fibrin clot. An experimental study in dogs.
Failure strengths of different meniscal suturing techniques.
Second look arthroscopy after meniscal repair. Factors affecting the healing rate.
Long-term results of arthroscopic meniscal repair. An analysis of isolated tears.