(See also: Plafond Menu)
Timing of Open Reduction
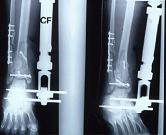
- in some cases, the fibula can be anatomically reduced along with application of external fixator which allows the fracture to be brought out to length and which allows the talus to be centered under the tibia;
- then 7-21 days later, medial column and articular surface can be restored once soft tissues have healed;
Incision
- use the CT scan and available radiographs to help determine the most beneficial location of the incision (as based on location of most displaced frx fragments);
- this should allow visualization and reduction of frx fragments, as well as bone grafting of the metaphysis;
- if possible, convert complex nondisplaced frxs in to more simple frx by inserting percutaneous screws across the major frx lines;
- in about 50% of patients, the incision will have to be biased anterolaterally, whereas in the remaining 50% the incision is biased anteromedially;
- anterolateral incision should be placed distance of at least 7.5 cm from lateral incision over the fibula to avoid skin slough;
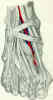
Anteromedial Approach to the Distal Tibia
- proximally incision is made 1 cm lateral to anterior tibial crest which places the incision over the anterior compartment;
- incision should be well lateral to subcutaneous surface of tibia;
- incision is carried longitudinally down to the level of the ankle joint, at which point the incision is carried either medially or laterally to allow exposure of the ankle joint;
- more often incision is carried medially (along medial aspect of tibialis anterior tendon at level of the ankle joint) to end just anterior to medial malleolus;
- care is taken not to injure the paratenon of the tibialis anterior;
- more often incision is carried medially (along medial aspect of tibialis anterior tendon at level of the ankle joint) to end just anterior to medial malleolus;
- alternatively, an incision is made from distal to proximal along the anterior border of the medial malleolus and upward in a straight line 1 cm lateral to crest of the tibia;
- dissection is carried through subQ fat in line w/ incision;
- if the plate is to be applied medially then the incision may need to wrap aroung the medial malleolus, where as if the plate is to be applied more anteriorly, then the incision should follow the medial border of the tibialis anterior;
- flap is not created between subQ layer & extensor retinaculum, rather the dissection needs to be deep to the retinaculum;
- cut is made distally to periosteum and more proximally medially through extensor retinaculum and periosteum;
Anterolateral Approach
References
- Reduction strategies through the anterolateral exposure for fixation of type B and C pilon fractures
- Bohler incision: an extensile anterolateral approach to the foot and ankle
- Surgical fixation of pilon injuries: a comparison of the anterolateral and posterolateral approach.
Lateral Incision
- kept posterior to most prominent portion of lateral malleolus & fibula, surgeon being concerned to keep as wide bridge of skin as possible between it & medial incision;
References
- Open Reduction and Internal Fixation of Tibial Pilon Fractures Using a Lateral Approach
- Staged Posterior Tibial Plating for the Treatment of Orthopaedic Trauma Association 43C2 and 43C3 Tibial Pilon Fractures
Posterolateral Approach
References
- Staged Posterior Tibial Plating for the Treatment of Orthopaedic Trauma Association 43C2 and 43C3 Tibial Pilon Fractures
- Posterolateral approach for tibial pilon fractures: a report of two cases
- A surgical approach to posterior pilon fractures
- Surgical fixation of pilon injuries: a comparison of the anterolateral and posterolateral approach.
Deep Dissection
- care is taken to preserve paratenon of tibialis anterior tendon;
- this is important because if skin problem develops, paratenon will accept skin graft while the tendon itself will not;
- tendon may become dessicated and lead to further problems in wound coverage;
- proximally, incision enters anterior compartment & then dissection is carried medially between anterior tibial musculature & anterior fascia to the periosteum
- subperiosteally elevate periosteum along with the medial skin;
Exposure of Frx Site
- minimal periosteal stripping is carried out;
- frx is displaced open w/ dental pick, to allow better visualization of the deep articular surface;
- temporary fixation of the articular surface is achieved w/ K wires;
Subsequent Steps
- restoration of tibial articular surface
- bone grafting
- implants for pilon frx
- cancellous bone grafting of metaphyseal defect
- wound closure