 - See:
- See:
- Diabetes Menu
- AliMed - diabetic resources
- Pathological Conditions:
- natural history leads to autonomic dsyfunction (loss of skin pliability), motor changes lead to altered wt bearing forces on the foot, and sensory dysfunction leads to formation of skin breakdown and wounds (leading cause of amputation);
- vascular pathology
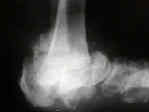
- diabetic charcot foot and ankle
- neuropathic ulceration
- ankle fractures in diabetics:
- main pitfall is failure to mistake an early charcot ankle fracture for a "simple ankle fracture;"
- failure to consider a charcot ankle fracture may lead to disasterous consequences for the surgeon and patient;
- in the study by McCormack and Leith (1998), the authors noted a 42% complication rate in the treatment of diabetic ankle fractures vs no complications in a match series of ankle frx patients without diabetes;
- of 19 patients treated surgically, 6 developed major complications, and two patients required amputation;
- diabetic patients w/ displaced ankle fractures treated non op showed a high incidence of loss of reduction and malunion but these caused few symptoms;
- the authors recommend strong consideration of non operative treatment in these patients;
- take care to apply generous padding to the cast in order to avoid pressure ulceration;
- Steinman Pin Augmentation:
- Steinmann pins placed across the ankle and subtalar joints to augment fixation and to prevent collapse;
- pins are left in place for 6-8 weeks;
- Ankle fractures in diabetics. Complications of surgical management
Examination of the Diabetic Foot and Ankle
- Diabetic Foot Infections:
- management of cellulitis or infected superficial ulcerations:
- see Wagner grading system for diabetic foot infections:
- non operative treatment is indicated for patients who are not septic, ie, no high fever, normal WBC, no altered mentation;
- cultures from ulcers are unreliable (need to treat based on deep cultures obtained from researach studies);
- enterococci may be most common and therefore a logical starting medication would be augmentin or unasyn;
- management of deep infections:
- osteomyelitis in the diabetic patient:
- immediate surgical debridement is indicated for all patients who appear acutely toxic (wet gangrene);
- be especially careful of the patient with pain/skin changes on both the dorsum and plantar surface of the foot;
- these patients will need both dorsal and plantar incisions for adequate debridement;
- note the depth and extent of the wound since this helps determine the extent of debridement;
- debridement not only decreases bacterial count but also decreases matrix metalloproteinase);
- be especially aggressive to remove devitalized fascia;
- goal is to remove devitalize tissue which interfere with wound healing;
- chronic inflammatory chages are coverted to an acutely clean wound;
- amputations in the diabetic patient
- compartmental anatomy of the foot
- wound dressings
- wound vac
- ref: Experience with the vacuum assisted closure negative pressure technique in the treatment of non-healing diabetic and dysvascular wounds
- Diabetic Neuropathy:
- cymbalta
- neurontin
- lyrica
The diabetic foot: evolving technologies.
Management of the diabetic foot.
Simplified two-stage below-knee amputation for unsalvageable diabetic foot infections.
One-stage versus two-stage amputation for wet gangrene of the lower extremity: a randomized study.
Ankle fractures in diabetics. Complications of surgical management.
Antimicrobial Management of Foot Infections in Patients With Diabetes Mellitus
- references:
- Treatment of resistant ulcers on the plantar surface of the great toe in diabetics.
- Management of diabetic midfoot ulcers.
- Diabetic foot infections. Bacteriologic analysis.

