Discussion
- arises from median nerve, 5 cm above medial epicondyle;
- runs on volar surface of FDP and along interosseous membrane between ulna & radius;
- supplies FPL, lateral half of FDP, & pronator quadratus;
- may supply sensory branches to distal ru and carpal joints;
- variations:
- martin gruber anastomosis occurs in 10-15% of all forearms and in half of these cases, the nerve communication arises from the AIN branch;
- hence palsy of the AIN could lead to palsy of the hand intrinsics normally supplied to the ulnar nerve;
- diff dx: FDP avulsion
Anatomy
- AIN is principally a motor nerve;
- it arises from median nerve at a variable point as it passes between two heads of the pronator teres, descends vertically in front of interosseous membrane between
FDP & FPL, supply these 2 muscles, & finally terminates in pronator quadratus near wrist joint; - it divides from the median nerve 4 to 6 cm below the elbow;
- points of compression:
- as it passes between 2 heads of pronator teres;
- deep head of pronator teres;
- as it descends vertically in front of interosseous membrane between FDP & FPL;
- orgin palmaris profundis
- gantzer's muscle (accessory head to FPL)
- origin FDS
- origin of FCR;
- thrombosis of ulnar collateral vessels;
- median artery
Exam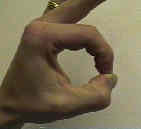
- principal weakness: difficulty moving index & middle fingers;
- weakness in flexors of ip joint of thumb (FPL) & dip joints of index and middle fingers - FDP;
- this can be observed by observing pitch attitude of the hand;
- normally when individual pinches something between index finger & thumb, MP & IP joints of thumb and index finger are flexed;
- w/ nerve deficit, terminal phalanges of thumb and index finger are extended or hyperextended;
- note:
- unusual innervation patterns of hand will confuse picture;
- median nerve hand (martin gruber) anastomosis:
- entire hand is innervated by the median nerve
- cross over ulnar innervations of FDP
- superficial innervations by anterior interosseous nerve;

EMG: needle examination is difficult because of the deep location;
Causes of anterior interosseous nerve compression:
- tendinous origin of deep head of pronator teres (most common);
- enlarged bicipital tendon bursa may impinge AIN;
- aberrant or thrombosed radial artery in midforearm;
- thrombosed ulnar artery;
- fascial band at the origin of FDS;
- compression w/in deep palmar compartment from aberrant accessory muscles such as FPL (gantzer's) muscle, palmaris profundus mass, or enlarged ? FCR brevis;
Diff Dx
- lateral cord lesion;
- FDP avulsion or avulsion of index profundus tendons;
- tendon ruptures are noted by placing digits in different positions and applying tension to the flexor tendons;
- electrical stimulation may indicates whether muscle belly is partially denervated;
- succinylcholine test: which may demonstrate more fasciculations of FPL if there is partial or complete denervation;
- in pts w/ low ulnar nerve injury, some interosseous muscle intrinsic function may be maintained due to martin gruber anastomosis between AIN nerve and unlnar nerve;
- C-8 radiculopathy:
- rare finding;
- the correct diagnosis is made by determining the function of the muscles innervated by the C-8 portion of the ulnar nerve;
- Parsonage-Turner Syndrome
References
- A simple clinical test to differentiate rupture of flexor pollicis longus and incomplete anterior interosseous paralysis.
- The anterior interosseous nerve syndrome.
- An anomaly of the median artery associated with the anterior interosseous nerve syndrome.
- Wrist Denervation and the Anterior Interosseous Nerve: Anatomic Considerations.
- Neurolysis is not required for young patients with a spontaneous palsy of the anterior interosseous nerve: retrospective analysis of cases managed non-operatively
- Brachial neuritis presenting as anterior interosseous nerve compression--implications for diagnosis and treatment: a case report
- Anterior interosseous nerve syndrome: retrospective analysis of 14 patients

