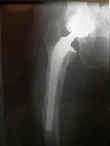
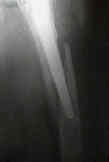
- See: Total Hip Replacement Menu:
- IntraOperative Frx:
- frx may occurr early while the attempt to dislocate hip is made;
- most postoperative femoral fractures can be prevented by avoiding injury to the bone during the original THR procedure;
- bone lysis from secondary aseptic loosening may significantly compromise strength of the femur and can lead to eventual frx;
- risk of intraoperative fractures with press fit stems:
- remember that many press fit stems inserted in elderly hip frx patients are often the cheaper designs compared to those inserted
in younger patients;
- press fit stems may by 14 times more likely to fracture than cemented stems;
- ref: Epidemiology of periprosthetic fracture of the femur in 32 644 primary total hip arthroplasties: a 40-year experience
- prevention of frx:
- osteotomy of the trochanter before dislocation may reduce the force necessary for dislocation and thereby reduce the risk of frx;
- fragile bone of elderly pts and of pts with RA or disuse osteoporosis may be frxd by moderate rotational force;
- when resistance is met in attempting dislocation in these pts, psoas tendon & more of capsule must be released;
- to dislocate hip posteriorly, partial transverse section of fascia lata & maximus insertion may be necessary as well as release of
tight, fibrotic band along posterior edge of medius;
- references:
- Increased incidence of femoral fractures in small femurs and women undergoing uncemented total hip arthroplasty - why?
- Intraoperative Proximal Femoral Fracture in Primary Cementless Total Hip Arthroplasty
- Frx Occurring in the Post Op Period:
- risk factors:
- inadequate calcar cancellous bone removal (w/ subsequent calcar resorption);
- varus positioning of the stem;
- lateral stem nicks produced by drilling for greater trochanteric wires;
- progressive osteolysis;
- small female patients:
- ref: Increased incidence of femoral fractures in small femurs and women undergoing uncemented total hip arthroplasty - why?
- Vancouver Classification:
- location, stability of the implant, and the surrounding bone stock
- type A:
- proximal fracture at the level of the trochanters;
- type B frx: fractures occurring at or near distal tip of a hip prosthesis
- type-B1 periprosthetic fractures:
- defined as a fractures occurring at or near the distal tip of a prosthesis with a stable femoral stem;
- associated with the most complications of all of the fracture types because of the inherently unstable fracture pattern;
- if component appears to be well fixed, consider leaving the prosthesis in place, and managing frx with a plate;
- proximal to the femoral component, the plate is secured w/ unicortical screws or with cerclage wires;
- note that sole reliance on locking plate may result in high rate of non union and/or hardware failure.
- references:
- Fixation of periprosthetic femoral shaft fractures adjacent to well-fixed femoral stem with reversed distal femoral locking plate.
- Locking compression plate fixation of Vancouver type-B1 periprosthetic femoral fractures.
- Locking plate osteosynthesis for Type B1 and Type C periprosthetic fractures of femur: a report on 12 patients.
- Surgical fixation of Vancouver type B1 periprosthetic femur fractures: a systematic review.
- Biomechanical Concepts for Fracture Fixation.
- type-B2:
- fractures occur in the same region with a loose stem
- short oblique frx at stemp tip: 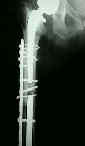
- arises due to a stress riser effect between prosthesis and bone;
- these frx are at high risk for displacement, shortening, & non union;
- not amenable to closed treatment;
- loose component:
- using large uncemented prosthesis & obtaining stability in diaphyseal region is often successful
treatment of these fractures;
- references:
- Locking compression plate fixation of Vancouver type-B1 periprosthetic femoral fractures.
- Locking compression plate versus revision-prosthesis for Vancouver type B2 periprosthetic femoral fractures after total hip arthroplasty.
- A systematic review of Vancouver B2 and B3 periprosthetic femoral fractures
- type-B3:
- fractures occur with a loose stem where the proximal bone is of poor quality and/or severely comminuted
- references:
- Classification of the hip.
- Periprosthetic fractures of the femur. An analysis of 93 fractures
- Treatment protocol for proximal femoral periprosthetic fractures.
- In Brief: Classifications in Brief: Vancouver Classification of Postoperative Periprosthetic Femur Fractures
- Vancouver B3 Fractures: Treatment Options and Tips.
- managment:
- management depends on frx location, fixation of the prosthesis, and amount of displacement;
- if the prosthesis is well fixed and if the fracture is minimally displaced, a trial of non operative treatment is indicated;
- femoral shaft perforations:
- bypass perforation by at least one and one half shaft diameters in order to reduce risk of shaft frx through perforation;
- clinical recommendations have been to use a femoral component that ends 2-3 shaft diameters distal to the perforation;
- proximal femur frx;
- frx usually cannot occur unless there is loss of fixation of proximal femoral component;
- frx may have produced disruption of the bone cement prosthesis interface or there may have been preexisting loosening;
- requires revision of the femoral component;
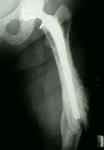
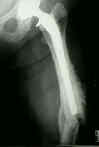
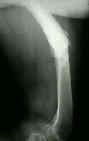
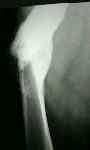
- example of femur frx occuring distal to the stem tip, which healed with use of traction and a cast brace;
- even though the fracture was angulated, the clinical result was good;
- long oblique frx at tip of prosthesis:
- more amenable to treatment in traction w/ subsequent cast bracing, if good alignment can be maintained;
- the main complication of non operative treatment is mal-alignment;
- bone distruction:
- w/ extensive bone destruction is such that large allograft is needed;
- femoral cortical allograft may be applied to the medial femoral cortex and is secured by a laterally applied plate;
- above the level of the prosthesis the allograft is secured w/ cerclage wires;
- medial cortical allograft is applied thru an extended medial approach;
- this treatment strategy often produces allograft healing by 5 months unless the patient has had previous
stripping the femoral periosteum in which case non union is possible;
- Cerclage Fixation Techniques: (from Cheng, et al (1993))
- Hairpin Cerclage Knot
- is significantly stronger than other fixation techniques;
- technique:
- wire is bent into a "U" shape;
- "U" is then passed around one end of the bone;
- one of the free ends of the wire is passed thru the "U" of the loop, and then the free ends of the wire are tension w/ a single
throw of a square knot;
- Harris Wire Tightener:
- single throw of a square knot is thrown and is then tensioned w/ the Harris wire tightener;
- wire is twisted 180 deg while under tension (more twisting may break wire);
- Harris tightener is released and final twisting is completed with pliers;
- references:
- A comparison of the strength and stability of six techniques of cerclage wire fixation for fractures.
Management of intraoperative femur fractures associated with revision hip arthroplasty.
Fracture of the ipsilateral femur in patients with total hip replacement.
The uncemented total hip arthroplasty. Intraoperative femoral fractures.
Femoral fracture during non-cemented total hip arthroplasty.
Treatment of proximal femur fractures associated with total hip arthroplasty.
The role of allografts in the treatment of periprosthetic femoral fractures.
Three Hundred and Twenty-one Periprosthetic Femoral Fractures.