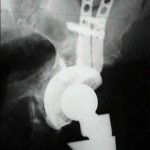
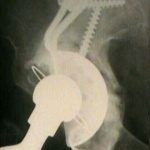
Discussion
- indications: salvage device for use in cases of pelvic discontinuity where a stable socket cannot be wedged between the anterior and posterior columns;
- classification of bone defects and bone grafting options:
- in almost every case, bone graft is morcelized and placed behind the cup;
- in many cases, structural bone grafting is required;
- ideally, the gap cup will protect the graft from weight-bearing loads allowing it to recreate continuity between the columns for future revision;
- this device is best suited for low demand patients;
- composition- pure titanium shell, 3 internal PMMA cement spacers to allow for consistent cement mantle
- template pre-op and draw cup in a position attempting to recreate native joint (avoid lateral displacement);
- confirm that cup size and appropriate cemented liner available;
- oblique films to identify columns;
- CT scan can also be helpful in cases;
- consider checking McCollum's line (sciatic notch to ASIS on standing lateral);
- lateral position, allow proximal wound extension if needed
component considerations
- thin plate attachments (2 mm or less) are prone to component failure;
- modularity
- reference:
exposure
- start laterally over femur coming proximally to a hand breadth above trochanter between ASIS, PSIS if using a trans-trochanteric approach;
- standard posterior approach incision except proximal aspect of wound should be slightly anterior to normal;
- a trochanteric osteotomy is generally not required unless the femoral component is not going to be revised thus necessitating more exposure;
- divide fasica lata in line with incision;
- stay within fascia proximally and avoid entering TFL muscle;
- dissect beneath fascia anteriorly and posteriorly;
- palpate sciatic nerve;
- consider finding nerve at gluteal sling if excessive scar prevents easy localization;
- if performing an osteotomy, identify anterior and posterior edges of gluteus medius, release short exterior rotators;
- perform osteotomy with gigli (proximal to distal) or oscillating saw (distal to proximal)
- lift gluteus medius sharply and with periosteal elevator;
- careful with notch;
- consider placing 2 Steinman pins in ilium for retraction;
- make sure proximal femur adequately released to allow anterior mobilization and place anterior acetabular retractor;
- outer wall of the ilium is cleared for several centimeters above the acetabulum;
- proximal lateral ischium is exposed for 2 to 3 cm, with care taken to avoid injury to the sciatic nerve.
removal of displaced acetabular component
- references:
- Multidisciplinary approach to revision of failed THR with significant pelvic discontinuity and intrapelvic protrusio of the femoral and acetabular components
- External iliac vein compression and thrombosis by a migrated acetabular screw following total hip arthroplasty
- Transperitoneal removal of an intrapelvic acetabular component after total hip replacement and salvage of a destroyed acetabulum
preparation and grafting
(see also: acetabular bone grafting)
- remove old cup usually with Smith-Peterson osteotomes.
- debride fibrous tissue with curet, acetabulum reamers to expose bone anteriorly and posteriorly.
- assess bone defects; (stressing inferior aspect of pelvis in an anteroposterior direction inorder to demonstrate motion at site of a pelvic discontinuity)
- palpate the superior ramus anteriorly and the ischium posteriorly;
- bone mill for allograft - 2 femoral heads or condyles;
- densely pack graft which by itself provides some structural support;
- place in acetabular bed and reverse ream with last size reamer used;
- make sure to dissect inferiorly to edge of obturator foramen (enough to get finger in);
- cauterize the branch from obturator artery;
component placement
- place component equal in size to the last reamer used with inferior hook just anterior to the ischium;
- rabbit ears should go proximally beneath medius along the ilium;
- the plates should not angle posteriorly near sciatic notch.
- gap cup position should similar to normal socket orientation or else impingement can be a problem;
- fixation sequence:
- dome screws are inserted first;
- place dome screws to pull the socket cephalad and atleast one screw in each rabbit ear;
- superior flange is fixed next;
- exposure of rabbit ears can be improved by placing an axial load on the femur pushing it proximally and retracting the medius anteriorly;
- ref: Cross-sectional Anatomy of the Ilium: Implications for Acetabular Component Placement in Total Hip Arthroplasty.
- inferior flange screws are inserted last;
- buttressing of the inferior pelvic bone stock is important to prevent component migration;
- ischial screw considerations:
- unicortical screws are not sufficient;
- need 2 bicortical screws, but 3 screws are better;
- sciatic nerve protection:
- careful dissection along the posterior column
- flex the ipsilateral knee and extend the hip inorder to relax the sciatic nerve;
- alternatively, the inferior flange can be inserted into a slot created in the ischium;
- at the junction of the ischium and the rim of the acetabulum, a slot is made for the inferior flange of the cage, initially using a high-speed bur or multiple drill holes;
- slot is then deepened and directed laterally;
- if a hook is present, use a bone tamp to seat the inferior hook then lock it in position with the crimper;
- reference: Neurovascular Injuries in Acetabular Reconstruction Cage Surgery. An Anatomical Study.
- cement augmentation:
- liner insertion:
- the liner should be about the same size as the gap cup;
- obtain XR - AP pelvis to compare cup location to other hip center;
- cement poly cup (can use an ordinary liner but a cemented cup is probably better);
- cage is typically in a more verticle and retroverted position than optimal, and therefore be careful to obtain optimal 45 deg abduction and 20-30 anteversion;
- 1 bag cement (40 g), allow to get quite doughy and roll in ball;(see optimal cementing techniques);
- place in a completely clean and dry gap cup and compress with clean glove containing mick pad;
- plastic pads on gap cup insure adequate cement mantle;
- orient the liner with Mckee/Aufranc guide;
- remove excess cement with curet;
- reduce hip when cement hard;
- check stability and then complete femoral preparation;
- strong consideration should be given to using a stem with additional offset to decrease impingement risk;
- dome screws are inserted first;
Outcomes
- in the report by Winter E, et al (2001), the authors evaluated 41 patients that required revision acetabular fixation with a Burch-Schneider Ring for acetabular defects;
- acetabular defect classified as type III or IV;
- morselized cryopreserved allogeneic cancellous bone graft was applied beneath the component;
- 38 hips were available for clinical and radiographic follow-up examinations at an average of 7.3 years after surgery;
- all measured clinical parameters had improved significantly by the time of the follow-up examination (p < 0.0001);
- radiographs confirmed that none of the 38 hips had any measurable migration or displacement of the acetabular component and that osseous consolidation occurred only within the grafted area in all patients;
- Allogeneic cancellous bone graft and a Burch-Schneider ring for acetabular reconstruction in revision hip arthroplasty.
References
- Use of reconstruction rings for the management of acetabular bone loss during revision hip surgery.
- Revision arthroplasty using an anti-protrusio cage for massive acetabular bone deficiency.
- Don't throw away the ring: Indications and use.
- Acetabular revision: The role of rings and cages.
- Technical factors for success with metal ring acetabular reconstruction.
- Acetabular revision with impacted grafting and a reinforcement ring: 42 patients followed for a mean of 10 years.
- The Burch-Schneider antiprotrusio cage in acetabular revision surgery: A mean followup of 12 years.
- The Burch-Schneider anti-protrusio cage in revision total hip arthroplasty: Indications, principles, and long-term results.
- Allogeneic cancellous bone graft and a Burch-Schneider ring for acetabular reconstruction in revision hip arthroplasty.
- Revision cup arthroplasty using Burch-Schneider anti-protrusio cage.
- Reconstruction of segmental defects during revision procedures of the acetabulum with the Burch-Schneider anti-protrusio cage.
- Acetabular revision with the Burch-Schnieder antiprotrusio cage and cancellous allograft bone.
- Ganz reinforcement ring for reconstruction of acetabular defects in revision total hip arthroplasty.
- Revision total hip arthroplasty with the use of structural acetabular allograft and reconstruction ring: a case series with a 10-year average follow-up.
- Reconstruction rings and bone graft in total hip revision surgery.
- Antiprotrusio cages for acetabular revision.
- Acetabular revision with impacted morselized cancellous bone graft and a cemented cup in patients with rheumatoid arthritis: three to fourtween-year follow-up.
- Complications of ilioischial reconstruction rings in revision total hip arthroplasty.
- Technical factors for success with metal ring acetabular reconstruction.
- Addressing severe bone deficiency: what a cage will not do.
- Acetabular Cages: A Ladder Across a Melting Pond
- Acetabular Rings in Revision Total Hip Replacement