- See: Bone Tumor Menu
- Discussion:
- benign osseous tumor usually less than 1.5 cm in diameter, comprising 11% of all benign bone tumors;
- no cases of malignant transformation has been reported;
- occurs primarily in adolescents and less often in children;
- it is rare in patients over age 40 yrs;
- presenting symptom is well localized pain which may be more severe at night & is relieved by aspirin or other prostaglandin inhibitors;
- because osteoid osteoma is a vascular tumor, substances which cause vasodilitation such as alcohol may precipitate an acute pain crisis;
- location:
- most common site is proximal femur, & diaphysis of long bones;
- less often: foot (talus, navicular, or calcaneus) & in posterior spine
- osteoid osteoma of the spine:
- may be an occult lesion;
- most often located in the posterior elements;
- may not produce a bony reaction;
- may lead to painful secondary scoliosis.
- bone scan is a useful test;
- references:
- Computed tomography of axial skeletal osteoid osteomas.
- Osteoid-osteoma and osteoblastoma of the spine.
- Osteoid osteoma of the spine. BA Arbarnia et al. Orthop. Trans. Vol 6. 1982. p 43.
- hand: diff dx: osteomyelitis, AVN, synovitis, TB, and RA;
- Exam: note whether there is a palpable lumb of reactive bone;
- Radiographs:
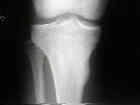
- intense bony rxn to small nidus is hallmark of osteoid osteoma, however, may be difficult to see on x-rays;
- look for oval radiolucent nidus only 3-5 mm in diameter which surrounded by disproportionally large, dense reactive zone;
- although usually located in cortex, nidus may occur subperiosteal and endosteal regions;
- Radiographic Diff Dx:
- Garre's osteomyelitis (chronic sclerosing osteomyelitis)
- Brodie's abscess
- Stress fracture

- Synovial herniation pits (Pitt's pits)
- common lesions in individuals with femoroacetabular impingement;
- tumor simulators and are incidentally identified on radiographs
- references:
- Herniation pit of the femoral neck.
- Symptomatic herniation pits of the femoral neck: anatomic and clinical study.
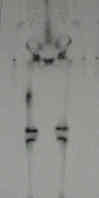
- Bone Scan:
- bone scans usually shows moderate or intense radioisotope uptake;
- CT Scan:

- nidus is best localized w/ CT - tell radiologist of diff dx:
- cuts should be 1-2 mm to visualize the nidus
- the window settings of the CT scanner should be adjusted so that
the dense reaction around the lesion does not obscure the
small low density nidus;
- MRI
- generally MRI has little role in making the diagnosis, because bone has a low signal;
- despite this, it can be used to confirm the diagnosis or to help rule out other lesions;
- Histologic Examination:
- nidus composed of thick vascular bars of osteoblastic tissue surrounded by vascular fibrous tissue finally surrounded by mature reactive cortical bone;
- Differential Dx:
- Osteoblastoma;
- is usually larger than osteoid osteoma;
- osteoblastoma usually does not produce an intense bony reaction;
- Osteosarcoma:
- Treatment:
- osteoid osteoma may resolve spontaneously w/ time (especially when located in the hand), however, most patients prefer not to
wait 2 to 4 years for resolution;
- when nidus is located in a low stress area such as metaphysis, treatment should consist of en bloc excision w/ surrounding small
block of reactive bone;
- tetracycline localization:
- using tetracycline at a dosage of 4 mg/kg, four times daily, 2 days preoperatively, the nidus will have a golden yellow fluorescence;
- the OR must be dark inorder to see it;
- percutaneous radiofrequency coagulation:
- involves percutaneous insertion of a biopsy needle under CT scan guidance;
- a tissue biopsy is taken in order to prove that the needle is properly located;
- then a radiofrequency electrode with a 5 mm exposed tip is introduced thru the cannula;
- the electrode is connected to a radiofrequency generator which raises the temperature of the tip to 90 deg C (which is
maintained for 6 minutes);
- as noted by Rosenthal et al 1998, results of this technique are comprable to the standard open technique;
- other options include, shaving of overlying margin of reactive bone until nidus is visible as red spot that can be removed w/ curettage;
- ensure that 1-2 mm of normal bone is curretted out as well
Subungual Osteoid Osteoma of the Distal Phalanx of the Great Toe
Osteoid-osteoma: intraoperative tetracycline-fluorescence demonstration of the nidus.
Osteoid osteoma. The double density sign.
Osteoid osteoma. Diagnosis, localization, and treatment.
Medical management compared with operative treatment for osteoid-osteoma.
Minimally invasive surgery for osteoid osteoma of the proximal femur.
Staging and treatment of primary and persistent (recurrent) osteoid osteoma. Evaluation of intraoperative nuclear scanning, tetracycline fluorescence, and tomography.
Osteoid osteoma diagnosis and management with low morbidity.
Osteoid osteoma: 95 cases and a review of the literature.
Osteoid osteoma of the proximal femur: new techniques in diagnosis and treatment.
Osteoid-osteoma: Diagnostic problems.
Percutaneous radiofrequency coagulation of osteoid osteoma compared with operative treatment.

