- See: Anterior Plate Fixation Methods
- Indications:
- open book pelvis injury w/ greater than a 2.5 cm pubic diastasis;
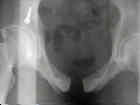
- note that fixation of pubic rami fractures can be much more complex than the fixation of a
simple diastasis;
- controversies:
- posterior injury and need for SI joint fixation
- failure to recognize posterior injury is a major cause for anterior plate fixation failure;
- urinary injuries:
- management of anterior symphyseal injuries w/ concomitant urethra injury:
- consider anterior plating of symphyseal injuries at either the time of supra-pubic catheter
insertion or within a 24-48 hour windonw;
- after 48 hours, risk of infection is unacceptably high;
- Preoperative Considerations:
- ensure that bladder and urethral injury has been considered;
- repairs can be performed by a urologist using the same exposure prior to symphyseal reduction;
- Open Surgical Approach:
- pt needs to be positioned supine on flouro table;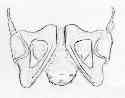
- be sure that the flouro machine can visualize the pubis;
- often the patient needs to be moved downward on the flouro table;
- Pfannenstiel incision:
- indicated when the fracture is located medial to the iliopectineal eminence;
- fractures lateral to this prominence endagers the vascular sheath, thru the Pfannenstiel approach;;
- in this case, use the ilioinguinal approach, which is indicated for superior ramus frx lateral to
iliopectineal eminence;
- transverse incisions offer execellent visualization;
- horizontal incision about 15-20 cm in length and 2 cm above symphysis;
- at the lateral edges of the incision take care to avoid the spermatic cords (or the round ligament in females);
- verticle incision:
- is an alternative to the Pfannenstiel, in cases of concomitant abdominal trauma;
- identification of the rectus:
- normally, the rectus abdominus muscle tendons insert onto the anterior aspects of the pubis.
- in acute case, rectus abdominis muscle has usually been avulsed and dissection is easy;
- in chronic cases this dissection can be very difficult because of scar;
- if the rectus has not be avulsed, then incise it, leaving a cuff of tissue attached to the pubis for later wound closure;
- alternatively consider a verticle incision between the halves of the recti muscles, leaving the muscles attached to the pubis;
- ref: [Refixation of the M. recti abdomini on the symphysis in traumatic pubis symphysis disruption. Reconstruction to the original anatomic situation].
- identification of the spermatic cords (and inferior epigastric artery):
- the dissection proceeds laterally, until the external inguinal rings and the spermatic cords are identified;
- ref: Anatomic relationship between the spermatic cord and the pubic tubercle: are our clamps injuring the cord during symphyseal repair?
- exposure of symphysis:
- identify the pubic eminences on either side of the symphysis;
- the anterior portion of the symphysis is cleared of soft tissue;
- ref: Does Removal of Symphyseal Cartilage in Symphyseal Dislocations Have Effect on Final Alignment and Implant Failure?
- hazards:
- surgeon must stay on the skeletal plane to avoid injury to bladder;
- the bladder lies directly behind the symphysis pubis, and in males the bladder neck is attached to the posterior surface of
pubis by puboprostatic ligaments;
- females in contrast, have a bladder that is in more contact with the pubococcygeal portions of the levator ani muscles;
- with previous surgery or an old injury, the bladder may be scarred to the undersurface of rectus & symphysis pubis;
- note proximity of symphysis both to spermatic cord & to NV structures;
- Reduction:
- reduction of the symphysis is usually easy in the acute case;
- assistant may apply pressure over each iliac crest or an external fixator can be applied;
- reduction clamps:
- orthomed pelvic reduction clampss
- Farabeuf and Lane clamps and large pointed pelvic reduction clamps;
- large pointed reduction clamps are applied into the obturator foramen and closed;
- large pointed reduction clamp can be placed onto each pubic tubercle or through holes drilled in the bone;
- expose the medial obturator foramen and application of pelvic reduction forceps thru the medial aspect of the foramen;
- alternatively two 4.5 mm screws are inserted into the anterior symphysis and farabeuf clamps are applied over these screws;
- external fixator can also be applied to assist with the reduction;
- hazards:
- during the reduction care must be taken to avoid trapping bladder or urethra in the symphysis when closing the clamp;
- ensure that the ends of the symphysis are opposed;
- surgeons gloved finger is passed into the space of Retzius;
- foley catheter is palpated (in the bladder) and continued urine output is noted;
- reference:
- A technique for reducing diastasis of the symphysis pubis.
- Anterior Plate Fixation Methods
Early failure of symphysis pubis plating.
Diastasis of the Symphysis Pubis: Open Reduction Internal Fixation
Implant retention and removal after internal fixation of the symphysis pubis.
Is fixation failure after plate fixation of the symphysis pubis clinically important?

