- Discussion: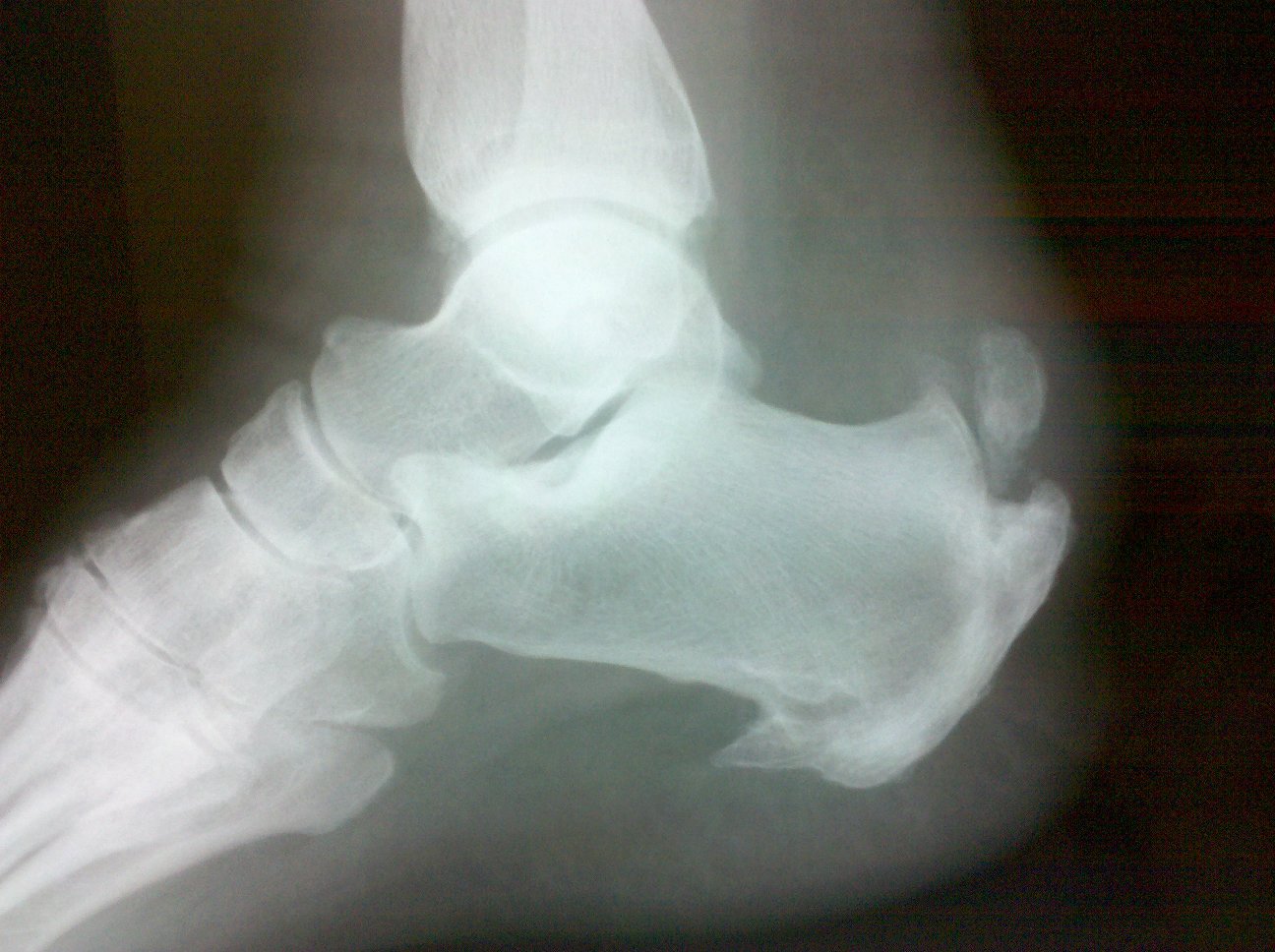
- inflammation can be related to a Haglund deformity (postero-superior prominence - normal varient) which causes an overlying bursitis;
- prominence of the posterior superior calcaneal tuberosity contributes to inflammation of the overlying tissues and the Achilles tendon;
- most often occurs in women and is related to shoe wear w/ rigid heels or heel counters;
- patients note posterolateral prominence and tenderness;
- diff dx: achilles tendinitis
- MRI:
- useful to determine if there are distinct degenerative areas within the tendon (achilles tendinosis), which might require debridement if resection of
the Haglund's deformity were indicated;
- Non Operativer Treatment:
- non operative treatment consists of heel cord stretching, change in shoe wear, NSAIDS;
- raising the heel out of the shoe with a heel insert, shifts the contact against the heel and often relieves symptoms;
- Operative Treatment:
- excision of the Haglund prominence can be effective in chronic cases;
- excision must be kept proximal to the achilles insertion;
- lateral approach is easier but care must be taken to avoid sural nerve;
- medial incision may also be used;
- vertical incision is made 1 cm anterior and parallel to the medial border of the Achilles tendon, and down onto the calcaneus;
- posterior calcaneal tuberosity is removed, and the Achilles tendon is debrided and reattached using bone anchors;
- Achilles tendon is dissected subperiosteally at insertion of Achilles tendon (about 50% of the tendon is elevated) and calcaneal prominence is removed;
- average size of the excised fragment is 3 cm wide, 3 cm long, and 6 mm thick;
- calcium deposits are removed from the Achilles tendon if they are present;
- patients are immobilized for four weeks
Operative management of Haglund's deformity in the non athlete: a retrospective study.
Chronic retrocalcaneal bursitis treated by resection of the calcaneus.
Prominence of the calcaneus: late results of bone resection.
The Achilles tendon insertion is crescent-shaped: an in vitro anatomic investigation.
Surgery for retrocalcaneal bursitis: a tendon-splitting versus a lateral approach.

