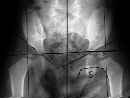
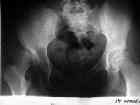
- See: DDH
- Indications for Radiographs:
- for confirming position of hips getting treatment;
- for confirming a suspected teratologic dislocation;
- Patient age:
- x-rays may not reveal a dislocation until infant is > 6 wks since so much of the pelvis is cartilaginous;
- in infants less than 3-4 months consider ultrasound if it is available;
- if ultrasound is not available, then consider obtaining two AP views, one view in adduction and one view in abduction;
- x-rays yield more reliable information when the child reaches 4-6 months of age;
- Characteristic Findings: 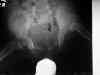

- increased acetabular index;
- provides useful information upto age 8 yrs;
- acetabulum becomes shallow incompletely developed (acetabular dysplasia);
- center edge angle
- provides useful information after the age of 5 years (may be used in adults);
- AP radiograph should be made standing w/ neurtal rotation;
- angle formed by a line drawn from center of femoral head to outer edge of the acetabular roof, and a verticle line drawn thru
center of femoral head;
- angles greater than 25 deg are considered normal;
- less than 20 deg indicates severe dysplasia;
- proximal & lateral migration of femoral neck adjacent to ilium;
- Hilgenreiner's Line: horizontal line along inferior aspect of triradiate;
- Perkin's Line: vertical line along lateral edge of triradiate;
- in infants less than 3-4 months the ossific nucleus will not be ossified;
- medial metaphyseal beak of the proximal femur should lie within the inner quadrant of the H and P lines;
- measure the distance of medial metaphyseal beak of proximal femur from H and P lines and compare this distance to the
opposite (presumably normal) hip;
- break in Shenton's Line:
- represents hip subluxation or dislocation as opposed to acetabular dysplasia;
- in pure dyplasia, this line will remain intact;
- appearance of Shenton's line can change w/ different degrees of rotation;
- delayed ossification of the ossification center of proximal femur;
- development of a false acetabulum;
- always consider presence of bilateral hip dislocation.
- accessory ossification centers:
- normal only 2-3% or normal hips have these centers, which tend to appear after age 11;
- in DDH, acetabular development may partiall occur thru these ossification centers;
- in patients that have been treated for DDH, upto 60% of patients will have accessory ossification centers
- they may appear as early as 6 months;
- Technique:
- accurate positioning is essential;
- hips must be extended & lower limbs in normal alignment & neutral rotation;
- Von Rosen View:
- used to evaluate femoral head reduction in child w/ suspected congenital hip dislocation/subluxation;
- pt is supine w/ hips abducted 45 deg & maximally internally rotated;
- AP projection of the pelvis is then obtained;
- ref: Diagnosis and treatment of congenital dislocation of the hip joint in the new-born.
- false profile view of Lequesne and de Seze:
- view best assesses anterior coverage of the femoral head.
- is obtained with the patient standing with the affected hip on the cassette, the ipsilateral foot parallel to the cassette, and the pelvis
rotated 65 degrees from the plane of the cassette;
- Clinical and radiographic assessment the young adult with symptomatic dysplasia.
- Arthrogram:
- note size of the limbus;
- capsular distension;
- medial pooling of dye;
- two directional arthrography:
- allows evaluation of the anterior, superior, and posterior portions of the limbus;
- lateral arthrogram not only allows visualization of anterior/posteror limbus but also allows visualization of iliopsoas muscle;
- types of limbus:
- everted: has a blunted and turned out appearance;
- intermediate: a blunted with and infolded shape causing minimal block to reduction;
- invereted: limbus is infolded and interposed between the femoral head and the acetabulum;
- the inverted limbus generally cannot be treated by closed means;
- in the study by Mitani et al (1997), 64 out of 137 hips with DDH had an inverted limbus on the AP arthrogram view, and 45 of
these hips had an interposed limbus on an anterior or posterior limbus;
- these authors noted that an inverted labram seen on any view would most likely prevent closed reduction
- Treatment of DD of the hip in children after walking age. Indications from two-directional arthrography.
Radiographic screening at four months of infants at risk for congenital hip dislocation.
The early identification and classification of growth disturbances of the proximal end of the femur.
Ultrasound screening for hips at risk in developmental dysplasia. Is it worth it?